Antibodies and COVID-19: What you should know
Editor's Note: This article was last updated on July 14 to include the most recent antibody testing numbers.
If you have a reasonably functioning immune system, your body regularly recruits and trains an army to fend off the invading pathogens it encounters. That is also the case for SARS-CoV-2, the virus that causes COVID-19.
So, let’s learn all about antibodies.

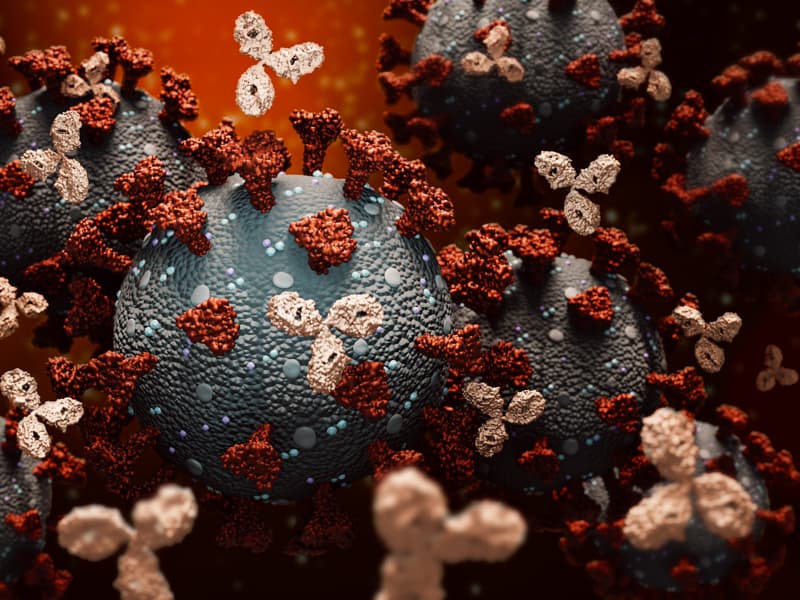
“Antibodies work to keep the virus from infecting new cells,” said Dr. Gailen Marshall, R. Faser Triplett Chair of Allergy and Immunology at the University of Mississippi Medical Center.
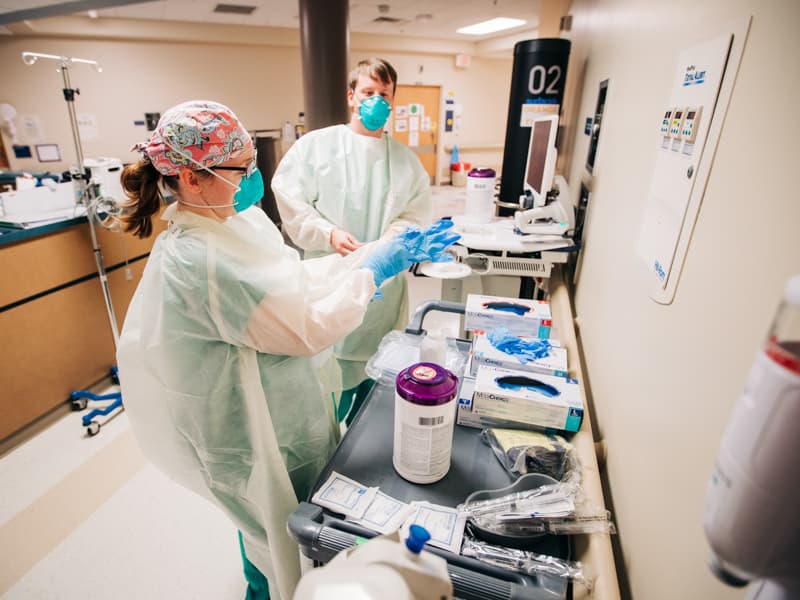
Clinicians use serology testing to show if someone has antibodies specific to a particular pathogen, such as the novel coronavirus that causes COVID-19. This blood-based test is different from the COVID-19 diagnostic test, which detects viral RNA from a nasal swab to confirm the diagnosis in patients with typical symptoms such as fever, chills, shortness of breath and cough.
As of July 14, UMMC had conducted 729 antibody tests. Thirty-nine came back positive. Statewide, there have been 13,793 antibody tests conducted by other health care clinics and Mississippi Blood Services, according to daily reports by the Mississippi State Department of Health.
So, what does it mean if your COVID-19 antibody test comes back positive? It tells you if you have antibodies or not, Marshall said, but nothing about the level of protection they provide.
“Having these antibodies does not make you bulletproof,” Marshall said.

“It does not mean that you are completely immune to this virus,” adds Dr. Ritesh Tandon, associate professor of microbiology and immunology. “It does not mean that you can go out in public without a mask.”
There is still a lot we do not know about the antibodies humans make in response to SARS-CoV-2. Tandon, who studies viruses, says that the antibodies our immune system makes against other coronaviruses can be detected for one to three years in blood. Since COVID-19 has been circulating for less than six months so far, we do not know where it falls in that range.
Furthermore, not all antibodies are created equal. Some viruses, such as HIV, elicit an immune response but the antibodies we make are not particularly effective at neutralizing this virus, Tandon said. We do not know enough yet about the characteristics of the COVID-19-related antibodies we produce. Immune response will also vary from person to person.
For instance, “Antibody levels are maintained through repeated exposure to their particular antigen,” Tandon said. “What I am seeing from the available data tells me that if you had severe symptoms after exposure to SARS-CoV-2, you may also have higher levels of neutralizing antibodies.”
To be clear, this does not mean people should expose themselves to people with COVID-19. With confirmed case counts and hospitalizations at record highs, the public still should wear masks, practice good hand hygiene and maintain social distancing.
However, there will be people who were exposed to and likely infected by the virus but had little or no symptoms, yet still produced antibodies and have some level of immunity. Identifying these cases will advance research into treatments and vaccines for COVID-19. Marshall, who leads a UMMC clinical trial testing of antibodies in plasma from people who recovered from COVID-19 can help currently-infected people recover, says determining the most-likely neutralizing antibodies requires studying their quality and quantity.
“A patient needs to produce both a sufficient amount of antibodies and the right kind of antibodies to be effectively immune,” he said, particularly antibodies targeting the spike protein this virus uses to enter cells.
Tandon and others at UMMC are studying the qualities and quantities of these antibodies in order to support the convalescent plasma clinical trial and develop useful biosurveillance assay profile. They recently finished a test of the latter, evaluating the University of Mississippi football team for the presence of SARS-CoV-2 antibodies.

Tandon describes the testing scheme as a “pyramid,” analyzing a subset of samples at each step to find the effective neutralizers. It starts with a commercially available test to show if antibodies are present or not. Next, the positive samples undergo an enzyme-linked immunosorbent assay, or ELISA, designed by Dr. John Bates, assistant professor of microbiology and immunology. This test shows how many antibodies are in a blood sample that can bind to the antigen: the coronavirus spike protein.
Finally, Tandon tests a subset of the ELISA-ed samples in a neutralization assay. He tests the antibodies against a pseudotype virus, which has proteins from the outside of SARS-CoV-2 coated over a different, non-pathogenic virus. Using the pseudotype limits the need for advanced biosafety measures and limits the risk of disease to investigators.
So far, “The assay is working and has been validated to some extent,” Tandon said. The team has been working on it for months, largely in-house and without outside contracts that would drive up costs.
The football survey showed that the percentage of players that tested positive for COVID-19 antibodies was comparable to the community-at-large, Marshall said. The Medical Center recently launched a similar study among UMMC employees to assess antibody prevalence between groups with different COVID-19 exposure risks.
“If we find that [a similar number] of our employees with high exposure risk have SARS-CoV-2 antibodies, then we can say that the measures we are taking to protect our employees are working,” Marshall said. “If it’s much higher, then we will need to improve our safety strategy.”

This study aligns with one of the most valuable uses of antibody testing at this stage of the pandemic, as “a way to assess SARS-CoV-2 infection within a population,” Dr. Larry McDaniel, professor and chair of the Department of Microbiology and Immunology, said in May. For instance, a health department could identify a community or group that may be spreading COVID-19 amongst themselves, then test a subset of those people for the antibodies to determine the extent of transmission.
But at the personal level, antibody testing has limited use at this point. If you want to go out and get an antibody test for your peace of mind, Marshall recommends asking the provider about the test’s specificity and sensitivity. Try to get a test where are least one of these values is at least 90 percent and the other is at least 80 percent.
“Having an antibody response is a good thing, and there is no reason to believe it is a bad thing,” Marshall said.
However, he repeats, “It does not make you bulletproof.”


