Homeless patient care focus of UMMC students' lesson

Pete Prince Jr. is a 60-year-old homeless veteran with an addiction and PTSD. Today he’s having trouble breathing. He’s well-known to the team at the University of Mississippi Medical Center’s Emergency Department, but today his usual COPD seems worse.
His nurses are concerned, as is his pharmacist, who found out Pete's prescriptions from his most recent ED visit last week were still in his shirt pocket, unfilled. His doctors think Pete needs to be admitted, but one of their colleagues, Dr. Paine, thinks Pete’s looking for a warm place to stay and isn’t really sick.
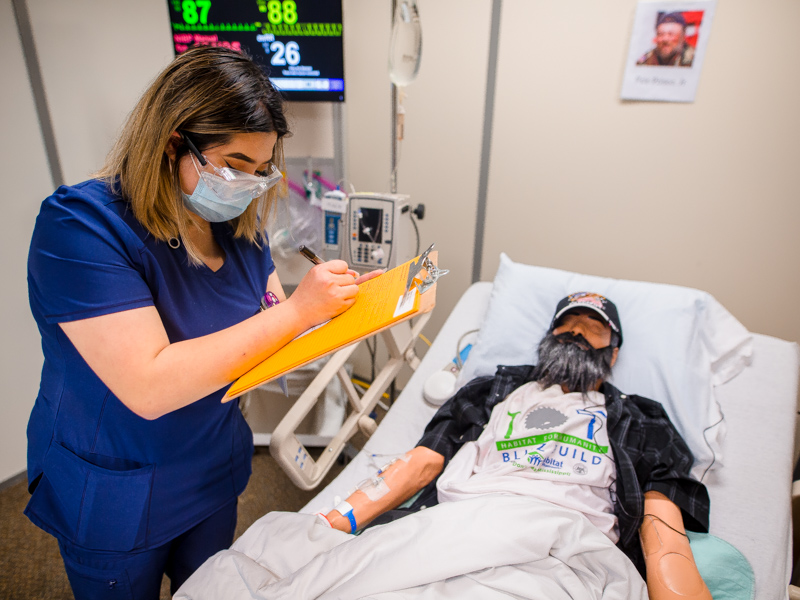
Pete is a simulation lab manikin at the School of Nursing at UMMC, and the role of Dr. Paine was played by School of Medicine faculty members in different simulations. On Thursday Pete’s doctors, nurses and pharmacists were UMMC students working together as a team to respond to this hypothetical situation as part of their training.

“We’ve been working by ourselves and with other nursing students, so this gave us the experience of working with other members of the care team,” said Madeline Nicosia, a junior working toward her Bachelor of Science degree in nursing.
Second-year medical student Jonathan Breaux said the simulation “showed the strengths other team members bring to the table.”

Pete has been a fixture at UMMC for more than a decade, said nursing instructor Hannah Hogg. “When I was a nursing student here, we would do simulated phone conversations about our patient, Pete. It has evolved quite a bit since then.”
Pete is now a manikin with the capability to let students hear his lung sounds. Members of the health care team noted wheezing in both lungs. Faculty members can be Pete’s voice, answering the questions his care team members ask. Pete has vital signs including blood pressure, which was a little high on Thursday, and an oxygen saturation that had dropped into the 80s, enough for his caregivers to recommend putting him on oxygen.
The aim of this annual exercise is for the interprofessional students to learn how to communicate with each other and their patient and become advocates for care.

“Each of you bring a slice to the table, but not the whole pie,” said Dr. Zeb Henson, associate professor of medicine, who debriefed teams of students after the simulations. “When you come together as a group, you will come closer to having the whole pie.”
Henson encouraged nursing students to communicate their concern or sense of urgency to physicians as well as a patient’s vitals. “Saying ‘I’m concerned about Pete,’ or ‘Pete comes in here often, but he looks sicker today,’ helps doctors triage what they need to do.”
Pharmacy students were coached on asking patients whether they have been taking their medications instead of assuming they are because prescriptions are listed in medical records. Offering suggestions to the team on less expensive prescriptions for patients was encouraged.
With no health insurance, Pete the manikin had been prescribed a list of medications that would have added up to $500 a month, according to his medical records, an amount that would be difficult for many people to pay out of pocket.
Students were also coached on making care conversations patient centered.
There’s a tendency for students to huddle together to discuss Pete’s condition instead of including Pete in the conversation, Henson said. Telling Pete that antibiotics are recommended will send the same message to the care team, who will get and administer the needed medications, “but Pete feels like he is a part of the discussion.”
Students were asked to consider the hypothetical Dr. Paine’s motivation. “He’s jaded,” said Breaux.
Others said maybe the fictional doctor who was set on showing Pete the door was burned out or, after caring for Pete often, had a case of care fatigue.
Showing the fictional doctor concrete evidence of Pete’s illness changed his mind, and Pete got the care he needed.
While Pete’s situation was hypothetical, health care professionals often encounter patients who are homeless in emergency-room settings.
“While this is a simulation, it is not unlike something students in nursing, medicine or pharmacy would encounter in an emergency room,” Hogg said. “In a year or two, these students will experience situations like this in real life.”
Through programs such as the Jackson Free Clinic and Dental Mission Week, the Medical Center works to help the estimated 1,352 Mississippians who are homeless or have financial challenges live healthier lives.
The Jackson Free Clinic is run by medical students at the University of Mississippi Medical Center in Jackson as well as volunteer physicians from the community. It offers non-emergency medical care, including evaluation, testing, prescription drugs and education, to individuals who cannot pay. Dental and psychiatric care are also offered. The clinic, located at 925 Martin Luther King Jr. Blvd., is open from noon-4 p.m. Saturdays.
The School of Dentistry, in partnership with schools across campus and volunteers from the community, provides free care for up to 300 patients a day during the annual Dental Mission Week. Each year, the effort results in free dental care for adults and children around the state who are underinsured or cannot afford dental care.


