Dental providers assess for oral health – and signs of sleep disorders
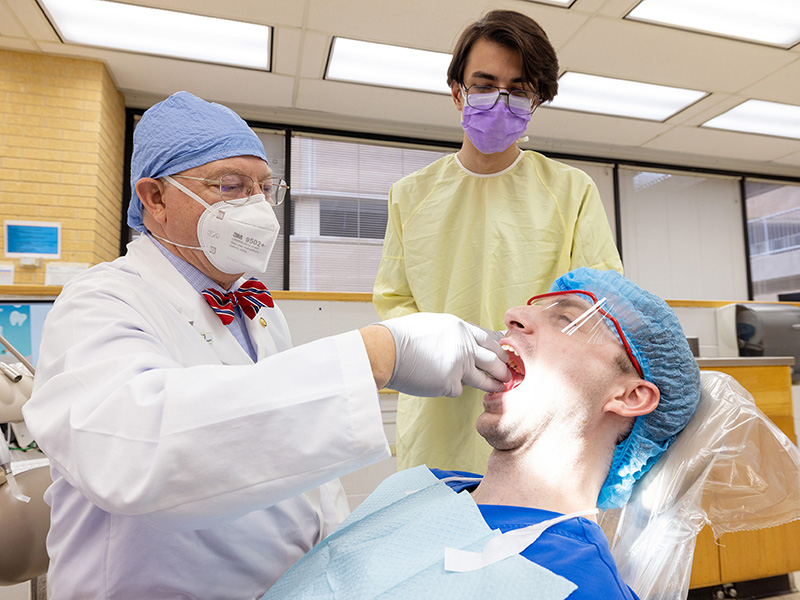
It was 2003. Dr. Bill Boteler had no idea how much of a toll bad sleep was taking on his body.
“My wife had been telling me, ‘You have been snoring so much. You’ve got to get tested,' remembered Boteler, an associate professor in the Department of Care Planning and Restorative Sciences in the School of Dentistry at the University of Mississippi Medical Center.

“I went in, and I was told I only had a mild case of sleep apnea. They said I didn’t need a CPAP,” short for continuous positive airway pressure, a treatment in which a patient breathes in pressurized air through a mask to prevent their airway from collapsing.
A year later, Boteler suffered a serious heart attack. “I got a stent the next day, and I became a heart patient,” he said.
His experience is one reason he is passionate about research into obstructive sleep apnea or OSA, a severe form of the disorder that occurs when the muscles supporting the soft tissues in the throat temporarily relax, narrowing or closing a person’s airway and momentarily cutting off their breathing.
“This has opened a new world for me on what dentists see, and what health concerns they can screen for in addition to sleep apnea,” Boteler said.
Left untreated, OSA can cause complications that include an increased risk of conditions that affect the heart and blood vessels such as hypertension, irregular heartbeat, heart failure and stroke.
“Sleep apnea is related to so many medical conditions. Oxygen deprivation is deadly, and we are learning more and more about that,” Boteler said. “When your airway is blocked, it’s a personal waterboarding experience. You wake up gasping for breath, like the bully held you underwater.
“That’s how it is for people with severe apnea.”
Boteler began teaching future providers how to screen for signs of sleep-related breathing disorders in 2016, when then-Dean Dr. David Felton asked for a faculty volunteer. “I thought, ‘If I had a heart attack related to it, I should teach it,’” Boteler said. “The more I learned about it, the more fascinated I was.”
SOD students and providers can screen for sleep apnea, but by law they can’t diagnose it. “If we see enough signs, we refer them to a board-certified sleep physician,” he said.

Dr. Andrea Lewis, a professor in the Department of Otolaryngology-Head and Neck Surgery, sees many SOD patients as part of the Medical Center’s multidisciplinary care.
“Dentists are in a unique position because they’re in the oral cavity to notice symptoms that correlate with sleep apnea,” Lewis said. “A lot of people with sleep apnea are tired and snore, but they don’t realize the correlation.
Boteler “has definitely been a huge advocate for screening patients in the community. I’ve gotten so many patients referred by him,” she said.
The American Dental Association advocates for the screening, as does the American Academy of Dental Sleep Medicine. “Many patients see their dentist more often than they do their primary care physician,” Boteler said.
There are dozens of signs and symptoms of obstructive sleep apnea. Just a few:
- A long uvula. “When the airway is partially blocked or collapsed, the uvula gets sucked into the trachea and gets beaten up as air is passing through a smaller opening,” causing someone to snore, Boteler said.
- A scalloped tongue. When someone has a fully or partially collapsed airway, the body attempts to reopen it by pushing the tongue hard against the teeth, making a scallop or impression on the tongue.
- Teeth worn down, broken or with chips in the enamel caused by clenching, gritting or grinding during sleep in an effort to reopen the airway.
- Acid reflux damage on teeth from when a patient struggles to breathe, causing the abdominal muscles to force acid up the esophagus and into the mouth.
- Abnormal shape of the palate or maxilla, too little space for a patient’s tongue, or pressure on joints caused by disorders of the jaw muscles.
“Not only does Dr. Boteler give his patients information, but he makes them feel excited about getting treatment,” Lewis said. “It makes his trainees excited about it.”

Third-year dental student Gunner Rhoden uses what he’s learned from Boteler to screen patients.
“Before coming to dental school, I had no clue that this was even in the realm of dentistry,” Rhoden said. “I see myself using this information after I graduate. It’s important as a medical professional to do as much as you can, within your realm and scope of knowledge, to help your patient.”
About 25 percent of SOD patients have sleep apnea, Boteler estimates. “It’s a big problem in Mississippi, and it’s so underdiagnosed,” he said.
“I can’t tell you the number of people he’s identified through screening,” Lewis said.
Dental providers also screen patients by asking if they have morning headaches, restless leg syndrome, get up multiple times during the night to urinate, are drowsy while driving, or have anxiety and depression, high blood pressure, trouble sleeping or low energy levels.
“It’s a relief when we explain that they might have a physical thing in their sleep causing the anxiety,” Boteler said. “If I have apnea, my body doesn’t know the difference between a terrorist grabbing me by my throat and cutting off my airway and my airway just collapsing on its own. My body just knows it’s short on oxygen if you gasp for air hundreds of times a night.”

Fourth-year dental student Jackie McGrath said she recently identified a patient with sleep apnea symptoms. The patient was referred to an ENT physician and is undergoing a sleep study, she said.
“It’s pretty quick and easy to do, and it’s important because a lot of other providers don’t look in the mouth,” McGrath said. “It’s kind of funny when you ask a patient if they are brushing and flossing, and then if they have dreams when they sleep. If they have dreams, they are in restful sleep, but if they’re no longer having dreams, that could be a symptom of sleep apnea.”
The Medical Center’s sleep medicine specialists and Ear, Nose and Throat (ENT) physicians who treat sleep disorders offer multiple treatments. In addition to CPAP, treatments include a surgically implanted device that delivers mild stimulation to the hypoglossal nerve that controls movement of the tongue and some airway muscles.
Some providers also offer a retainer-like appliance that fits over the upper and lower teeth via connecting arms. It keeps the jaw from dropping back and creating a blocked airway, Boteler said.
Boteler and the SOD are just beginning to teach dental hygiene students how to screen for symptoms of sleep apnea. “They’re usually the first one to see the patient. Dental hygiene is the perfect place to screen for this,” Boteler said.
“We tell all of our students that they should screen 100 percent of patients. Don’t let one of them get away without addressing it,” Boteler said.
“For the patient, it can be life changing.”

