Newest transplant surgeons women with a mission

Hundreds of Mississippians are coping with organ failure – and too often, dying prematurely – because chronic health conditions leave them no alternative but a life-saving transplant.
Two new University of Mississippi Medical Center surgeons, however, are intent on changing the statistics. They’re passionate about getting word of the state’s only transplant program to those most in need and educating them about why they’ve become ill.
“It’s about getting awareness out about our willingness to take care of these patients,” said Dr. Hannah Copeland, assistant professor of cardiothoracic surgery and the newest addition to UMMC’s heart transplant program. “There’s an under-appreciation, or underestimation, for what we can do here for heart failure patients in our state.”
Copeland and Dr. Felicitas Koller, assistant professor of transplant surgery, began work at UMMC in the second half of 2017. They’re among an estimated 15 percent of transplant surgeons nationally who are women, and Copeland is UMMC’s first woman faculty heart transplant surgeon. Koller, a liver transplant surgeon, is only UMMC’s second woman faculty abdominal transplant surgeon. Dr. Fauzia Butt was a UMMC kidney transplant surgeon before joining a hospital transplant practice in the Detroit area in 2014.
The two new faculty members have more in common than being dedicated to saving lives through transplant surgery. Both were recruited by UMMC surgeons who they got to know during their training.
Both are moms to two small boys – and both have spouses who are stay-at-home dads. Both are determined to educate their patients on their diseases, and to make them aware of how crucial it is to address early on what can lead to organ failure.
“Some people don’t go to their doctor because they think they’ll feel better tomorrow,” Copeland said. “People with heart failure learn to adjust their lifestyle to accommodate their symptoms. They go up the stairs less, or walk less. They wait too long to be treated.
“I want to raise awareness about patients coming in sooner, and their primary care physician referring them sooner, so that they can have the best outcome,” she said.
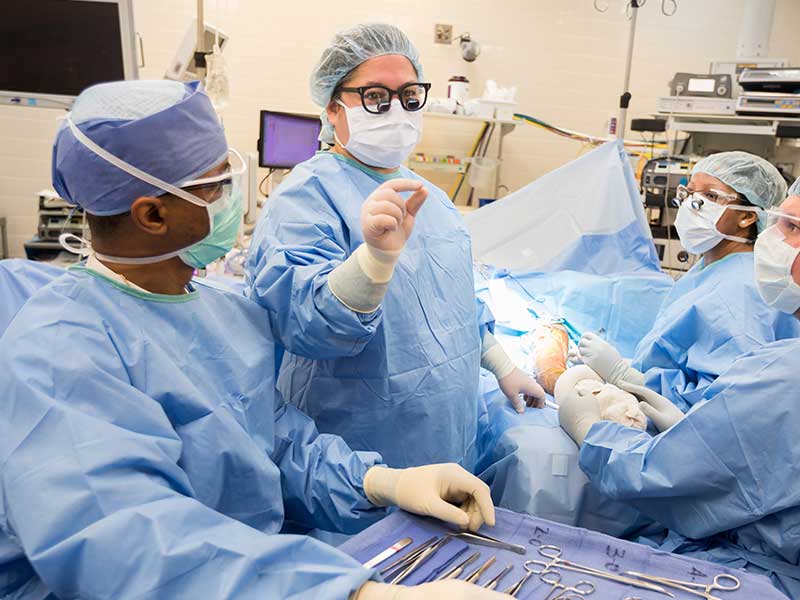
Koller acts as the “disease educator” for her patients. “So many of their problems are because of a failure of understanding their health,” she said. “I want to try to explain things to my patients in a way that they can understand what’s happening to them, why it’s happening to them, and what role they have in making positive changes. I try to empower them to have a say in their health.”
Copeland comes to the Medical Center from the McGuire Veterans Affairs Medical Center in Richmond, Virginia, where she was a cardiothoracic surgeon. A 2006 graduate of the University of Missouri-Kansas City School of Medicine, she was a general surgery resident and clinical research fellow at the University of Arizona, a general surgery resident at the University of California-San Diego, a cardiothoracic surgery resident at Loma Linda University, and a cardiothoracic surgery transplant fellow at Indiana University.
She’s certified by the American Board of Thoracic Surgery. In addition to heart transplantation, her major fields include mechanical surgical support, extracorporeal membrane oxygenation, or ECMO, cardiac critical care medicine and surgery education.
Before arriving at UMMC, Koller was an assistant professor of surgery in the Department of Surgery’s Division of Organ Transplantation at the Feinberg School of Medicine at Northwestern University in Chicago. She’s a 2005 graduate of the University of Texas Medical Branch in Galveston and completed her internship, a surgery residency and a surgical oncology research fellowship at Vanderbilt University in Nashville. She completed a multi-organ abdominal transplant fellowship at Northwestern Memorial Hospital, the academic medical center hospital for the Feinberg School of Medicine.
Koller is certified by the American Board of Surgery and received teaching awards for years 2013-2016 from Northwestern University’s Department of Surgery.
Copeland gravitated to surgery as a medical student because she was interested in “how surgical problems are handled – fixing a problem in the OR and then the patient improves,” she said. Vascular surgery initially interested her, Copeland said, but that changed when she gained exposure to cardiovascular surgery patients in the ICU.
“I was encouraged to pursue a year of research. That really allowed me to think about taking care of patients. It solidified my decision to go into cardiothoracic surgery,” she said.
“I’d always wanted to be a physician, and I thought I’d have a family medicine practice,” Koller said. “I absolutely fell in love with surgery because of the impact it could have on someone’s life, and the immediate difference a surgery can make. The first time I saw a patient get a liver transplant, I thought it was magical. I didn’t think it was possible for a person to go from so sick to so well.”
She met her husband George Koller, a physical therapist, and “with his support, I was able to muster up my courage and become a surgeon.”
Copeland trained with Dr. Jacob Moremen, UMMC assistant professor of cardiothoracic surgery, at Indiana University. She embraced the chance to work with Moremen and his team. “I like being at a university and the academic opportunities that come with that,” Copeland said.

“I knew Hannah would be a good fit here at UMMC because she has a great attitude and communicates well,” Moremen said. “She wholly invests herself in the care of her patients, and it shows.”
When Koller was an intern at Vanderbilt, the chief surgery resident was Dr. Christopher Anderson, UMMC professor and chair of the Department of Surgery. Also working at Vanderbilt then was UMMC’s Dr. Mark Earl, associate professor of transplant surgery.
“I’ve always had the deepest respect for both of them,” Koller said. Then, she met Dr. James Wynn, UMMC professor of transplant surgery, at a conference.
“When I saw the partners I could have at UMMC and the difference I could make, I thought it was amazing. I wanted to be a part of that,” she said.
Said Earl: “We are incredibly fortunate to have Dr. Koller join our team. She brings an impressive skill set, a wealth of transplant knowledge and positive energy to the team. Her addition will facilitate further growth of the program in both volume and complexity.”
Some of their new patient population is different than what they left – in Copeland’s case, only veterans treated at the Richmond VA, and for Koller, many from urban Chicago – but the demand for organs doesn’t change.
“The challenges people face are the same. The experience of illness is not any easier when you’re in the city or in a rural state,” Koller said. “All the people I cared for in Chicago had the same problems.”
What’s impressed her about Mississippi, Koller said, is the extended families and networks of support surrounding many patients. “I’m touched by people’s faith and the magnitude of their faith. It’s an honor to serve people who have lived through the time of Jim Crow, and to be of any assistance to the people who did so much for equality in the United States.”
Copeland, whose mother is Cuban and father is from Israel, has lived in cities in the Northeast, Midwest, Pacific Coast and in between. That’s making it easy for her to assimilate in Mississippi, she said. “There are a lot of good opportunities here for end-stage heart failure and lung failure treatment and programs to build.
“There are so many great and diversified places – different people, different cultures – and I’ve been fortunate to get to know them,” she said of moving around the country. “I appreciate that experience. It’s easier to help people if you know what their daily struggles are.”
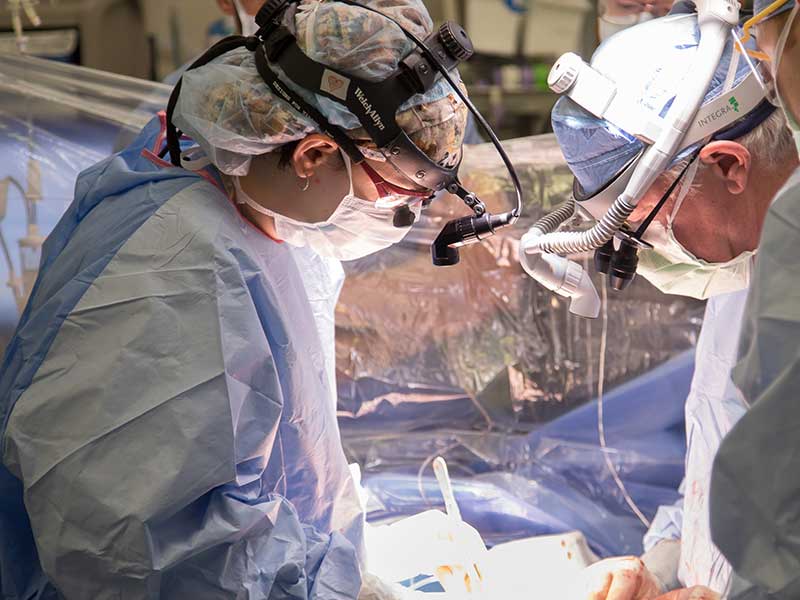
Copeland finds some of her heart and thoracic patients with chronic diseases could have avoided surgery if they’d taken better care of themselves. It’s a work area for her new patient base, especially in a state with staggering rates of obesity, heart disease, hypertension and diabetes.
She will be a catalyst for that change by working with the Mississippi Organ Recovery Agency and the organ donor community to promote early intervention for cardiothoracic diseases. “When a family member is touched by a heart attack, a transplant or an organ donation, that’s a better way to raise awareness than anything I can do,” Copeland said.
Copeland and Koller say they’re grateful for husbands who do the heavy lifting when it comes to chasing small boys.
In Copeland’s case, that’s retired physician Dr. Jack Copeland, a noted cardiac surgeon who helped pioneer the use of artificial hearts in the 1980s. Their boys are ages 7 and 5.
“I deal with it one day at a time,” she said of juggling family and work.
“It’s completely the whole key,” Koller said of her husband staying home with their boys, ages 4 and 2. “It’s allowed us to have a family in a way that we feel good about. It underscores how supportive my husband is of my career.”
It would be easy to come home and talk shop, Copeland said, but she doesn’t. “I might say what I’m frustrated about, and then we talk about the kids. We talk about homework,” she laughed. “We both have the same work ethic. He understands when I’m not there. He explains to the children why I might not be there, and he explains it well.
“When I get home, it’s about home,” said Copeland, who lives in Jackson. “I want to be mentally there. It’s not to anyone’s benefit for me to be half present, either at work or at home.”
Moving to Mississippi from Chicago has its perks, Koller said. Her sons, ages 2 and 4, delight in the next-door neighbor’s cows and donkeys. “We sit and eat breakfast and watch the cows parading by,” Koller said of the five-acre farm they now call home.
And, there are the cultural differences. “One benefit of the South is that people know how to dress a child,” Koller said. “When we go to the Children’s Museum, the bow is bigger than the little girl’s head.
“From the business that is my life, the things I really need in my life are Target, Whole Foods and Amazon Prime,” Koller said. “All those things are easy to get here.
“I live 10 miles from my office. In Chicago, I lived 10 miles from my office. It took me an hour and a half in the evening to get home. Here, it takes 20 minutes,” Koller said. “Living here has been so much easier. It’s been awesome.”

