Caring for COVID-19-positive moms a labor of love
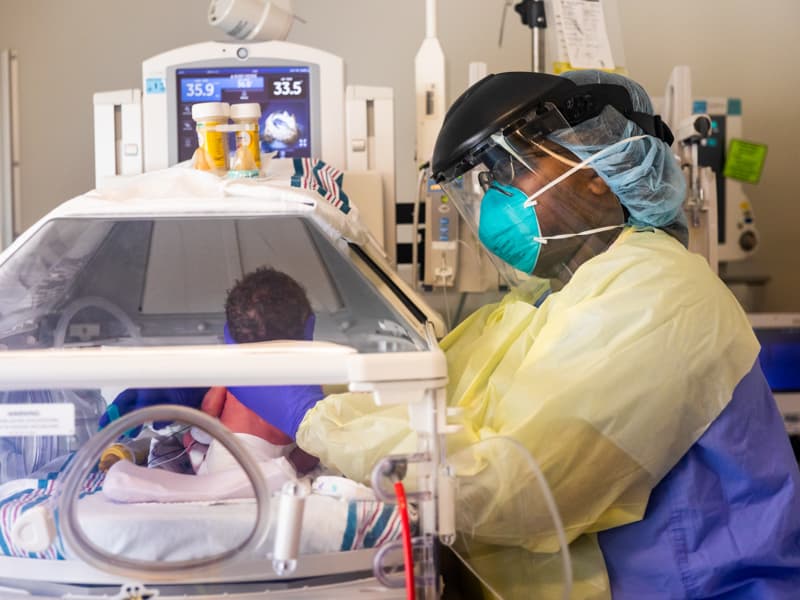
Dr. Rachael Morris remembers well the first pregnant woman positive for COVID-19 to give birth at the Winfred L. Wiser Hospital for Women and Infants.
It was April 14. The gravely ill expectant mother was in the medical intensive care unit, not on a ventilator, but receiving oxygen. Nurses carefully pushed her in her bed to one of the two Wiser operating rooms reserved for COVID patients.
After her baby was born via C-section, the young mother was wheeled back to the Conerly Critical Care Tower, about a five-minute walk from Wiser.
Because the baby was so close to term, “we moved toward delivery,” said Morris, a maternal-fetal medicine specialist and associate professor in the Department of Obstetrics and Gynecology at the University of Mississippi Medical Center.

The baby, born free of the virus but ill enough to need critical care, was whisked to the neonatal intensive care unit on the first floor of Wiser, UMMC’s hospital primarily devoted to women and newborns.
Although many COVID patients who end up in the ICU don’t survive, this mom and her baby did. Since that first delivery, about 56 COVID-positive moms have given birth at Wiser. All told, as of July 22, Labor and Delivery has cared for 92 COVID-positive women.
“Obstetrics in general is very unpredictable. COVID has presented a very unique situation,” Morris said. “An emergency from a fetal or maternal perspective can happen at any time with a COVID patient. Sometimes, you have seconds to intervene on a baby.”
Not one COVID-positive mom giving birth at Wiser has died. All of their babies have been COVID-negative.
Morris and Wiser’s Labor and Delivery team have worked hard to develop a rhythm of care, not just for COVID-positive patients, but hundreds of mothers and babies free of the virus who require their own specialized treatment.
Before COVID, mothers had their babies either through a C-section in a second-floor Wiser OR or down the hall in a Labor and Delivery birthing suite. Unless they needed a higher level of care, they’d go to the Mother-Baby Unit on the third floor following delivery.

Their babies would room in with them unless illness or complications required NICU care.
The highly contagious nature of COVID has given complex care in a very full women’s hospital a whole new meaning. The majority of mothers already are high-risk because of comorbidities including obesity, diabetes, sickle cell, HIV and hypertension.
COVID on top of that presents challenges and scenarios unlike any Labor and Delivery providers have seen, or might ever see. “Our numbers are rising quickly. It’s not slowing down,” Morris said.
“I’ve eaten, breathed and slept this since the week of spring break,” said Leslie Hood, a nurse educator who served as a Labor and Delivery nurse manager for most of the pandemic.
“Having to lead through a pandemic – to be the one to figure out the answers and to support the staff – that’s been an experience.”
‘We are so hands on’
Every day, providers must make a call on where to place moms before and after delivery. “It’s so complex. There are so many situations that come through our doors,” Hood said.
The patients include women receiving prenatal care from UMMC and those who haven’t received it anywhere. There are very sick mothers transferred from other facilities.
There are mothers in an obstetric emergency on top of COVID, or so sick from COVID that they must go straight to the ICU. Some might first arrive at the Adult Emergency Department or at Women’s Urgent Care. On the ground floor of Wiser, Women’s Urgent Care is for moms with obstetric emergencies, including early labor.

The truly sick moms “could go into respiratory failure,” said Dr. Marty Tucker, professor and chair of the Department of Obstetrics and Gynecology. “They can have pneumonia and high fever. The main thing that gets them into the hospital is the inability to breathe. They get fatigued and weak.”
Early in the pandemic, “we had six deliveries where the mother tested positive after delivery,” Hood said. “That drove us to universal testing for all mothers. If a mother comes in and delivery is so imminent that we can’t wait on a standard test, we do rapid testing.”
Those moms require a special Labor and Delivery room with filtering and ventilation that pushes potentially contaminated air outdoors. “Every second counts so far as staff exposure,” Hood said. “We get them into a negative pressure room as soon as possible.
“We are so hands on, and we are so diligent with our PPE. We have all of our other high-risk moms. We’re doing it all on the same unit.”

In mid-March, Hood and Morris began developing and test-driving protocols and processes for COVID-positive moms and their babies. Joining them were Connie Richardson, Wiser’s director of nursing; Yolanda Moore, a Women’s Urgent Care nurse manager; Nital Parrish, Labor and Delivery nurse manager; Dr. Mobolaji Famuyide, chief of pediatric neonatology; Dr. Amber Shiflett, medical director of Wiser; and Alice Chaney Herndon, Mother-Baby Unit nurse manager.
Tucker, who began work at UMMC Jan. 13, had barely had time to settle in. “He empowered us, and then asked us what we needed from him,” Hood said.
“At the time, there was no data out there. We mapped things out and practiced different scenarios – how to safely deliver them, how to transfer them and how to keep employees safe. We did simulations with Women’s Urgent Care.
“We rounded and talked to the staff to make sure they knew were going to do things to keep them safe,” Tucker said. “We wanted their input on how to make things better.”
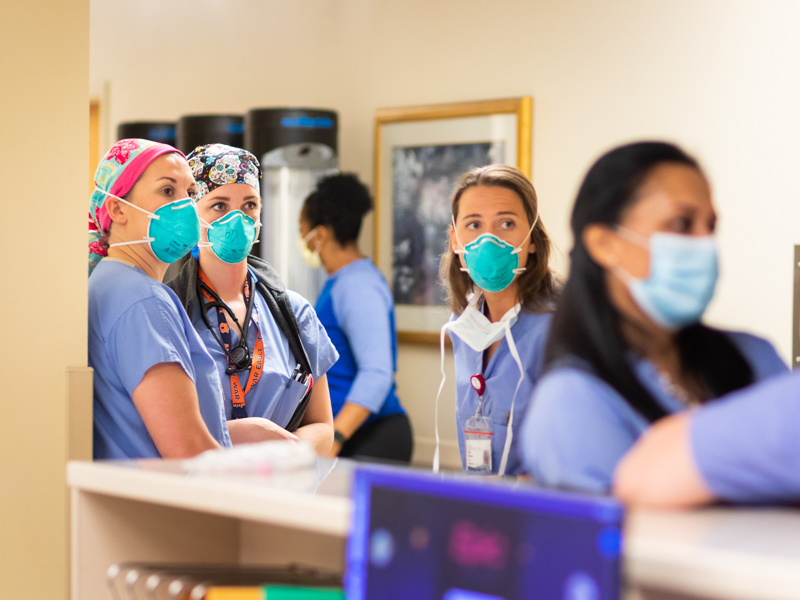
Morris said she worked closely with Dr. Andrew Wilhelm, medical director of the MICU, “to develop what an obstetrical care plan should look like. We created an emergency care C-section algorithm. We developed a surgery workflow and a multidisciplinary approach to care.”
On April 14, they were as ready as they could be. “We created a C-section simulation video to educate our caregivers based on that first case. We put it on YouTube to help educate other academic medical centers,” Hood said.
They pioneered a continuity of care for COVID-positive moms that stretches far beyond Labor and Delivery.
If a pregnant mom is in the ICU, Labor and Delivery staff come to her. “We’ve had our nurses hold the fetal monitors on these moms because they are coughing so hard,” Hood said. “Our nurses who work with them are rock stars.”
Post-delivery, COVID-positive moms go to University Hospital floors dedicated solely to COVID patients. A Labor and Delivery mother-baby nurse follows them.
It’s a deployment of resources that must be managed carefully. “We’ve had to do creative staffing to make sure our standard of care doesn’t change,” Hood said.
The COVID birth experience
If a pregnant mom is admitted and subsequently tests positive for COVID, “the entire birth experience changes in a second,” said Meredith Morris, a Labor and Delivery nurse.
“The first thing that happens is that the family member who is with them is sent home, and the mom is put into a negative pressure room,” Meredith Morris said. “When I tell them they’re going to be tested for COVID, I tell them the protocol so they won’t be surprised by it.
“A lot of the time, they’re more anxious that they have to be alone, and that the father of the baby can’t be there, than they are about the actual sickness. They don’t get to see their baby until they go home.”
Vaginal delivery is safer and preferred if the mother is well enough. As few people as possible are in the patient’s room during delivery, and the baby is taken to the NICU or a special isolation nursery.

But when a C-section is needed, seconds could count. “You don’t want to do an emergency C-section on a COVID patient. Anesthesia needs time to intubate them,” Hood said.
A small handful of pregnant moms have been taken from the MICU to Wiser to give birth, then returned to the MICU. It’s stressful and sad when a mom on Labor and Delivery deteriorates, and the decision is made to move her to the MICU.
“When you relieve excess fluid and decrease the size of the uterus, it can help turn that mom around,” Hood said of delivering the baby of a woman who’s desperately ill.
Before a COVID-positive mom undergoes a C-section, she is covered with a sheet and puts on a face mask. She’s wheeled out of her room by a “dirty team” in full PPE. A “clean team,” also in PPE, takes over and transports the patient to an OR. Meanwhile, the “dirty team” is changing into fresh PPE to receive the patient.
All told, the OR team includes an obstetrician, anesthesiologist, Labor and Delivery nurses, O-B scrub techs, residents and fellows. “The staff knows there’s no social distancing when you’re delivering one of these babies,” Rachael Morris said.

The patient is draped with a special plastic. “When we intubate, we are protecting people in the area from the patient’s respiratory droplets,” said Dr. Arthur Calimaran, professor and vice chair for education in the Department of Anesthesiology
“We do our best to make sure they’re awake and have a spinal” instead of general anesthesia, Meredith Morris said. “But if we need to, we will intubate.”
The new mom can’t touch her baby. “They’ll give us their phone, and we will take pictures for them,” Meredith Morris said. “We try to do as much as we can to make it a good experience and to keep it like a normal birth.
“It’s been so nice being here for the patients who don’t have anyone else here for them – to be their family member.”
Confidence and a knowledge base
Hood resigned her position for personal reasons, effective Feb. 11. “But then I realized it wasn’t a good time to leave,” she said.
“I had to make sure my patients and staff were successful. I had to make sure Nital was successful.”
“Her plans long before this happened were to step down, but she stayed the course,” Tucker said “It would have been so easy for her to leave, but when her staff saw her step back into the battle, it emboldened them even more.”
Rachael Morris is proud of the Labor and Delivery team – residents, fellow, faculty, nurses, support staff and others who have stepped up to care for a special group of moms and babies.

“Our teams are handling COVID with confidence and a knowledge base. I’m worried about the rise that is probably going to occur because of social gatherings. That’s why we’re seeing an explosion in numbers, and it will continue.”
Tucker has three main concerns. “We will see peaks and valleys over the next months, and we want to survive those peaks,” he said. “We don’t want to be over capacity. We can’t have everyone having COVID at the same time.
“My second area of concern is burnout of doctors and medical staff, including people who work in the ICU, in the ED, in the OR. Obstetrics is high volume and high risk, even in the best of times. We’ve had good planning to this point, but everyone has their breaking point.
“My biggest fear … We’ve been so fortunate that this virus hasn’t run through our staff and faculty. That could literally happen overnight. You could have 10 or 12 people go out for 14 days. There are no reinforcements behind them. We worry about the long-term health of people who work in health care. Some get low-down sick, and some die. Safety is an utmost concern.”
The Labor and Delivery staff has “respectful fear” for the virus, but are undeterred in staying the course on a pandemic with no expiration date, Hood said.
“They may have limped across the street going home, but came back the next day thinking about how they can better take care of their patients.”


