COVID-19 impacts black communities more heavily, study shows

United States counties with disproportionately black populations are experiencing more confirmed COVID-19 cases than other areas of the country, according to data released Tuesday.
The study shows that while about one in five counties are disproportionately black, these areas account for 52 percent and 58 percent of COVID-19 cases and deaths, respectively, in the United States.
“These findings not only resonate, but also call for reflection on the sad reality that as a nation, we have not made the public investment necessary to address the underlying forces that create and maintain these disparities,” said Dr. Leandro Mena, professor and chair of the Department of Population Health Sciences and professor of medicine at the University of Mississippi Medical Center.
Mena, a co-investigator for the study, joined some of his collaborators for a virtual news conference May 5. Researchers from the Foundation for AIDS Research, Emory University, Johns Hopkins University and Georgetown University also contributed to the study.
The paper, which is undergoing review for acceptance in a scientific journal, will be among the first to quantify racial disparities in COVID-19 infections and deaths on a national scale.

As of April 13, when the data used in the study was collected, “we did not have reliable national data on race and COVID-19,” said Gregorio Millett, vice president and director of public policy for the Foundation for AIDS Research and lead author of the study. “We were urgent to share the details of our study now in order to influence policy decisions.”
Millett said the study group also plans to run a similar analysis focused on COVID-19 in disproportionately Hispanic and Latino counties.
The study, which used U.S. Census Bureau and public health data, considered a county disproportionately black if more than 13 percent of residents identified as black or African American. Twenty-two percent of U.S. counties are in this category, and 90 percent of those are in the southern United States. In Mississippi, 76 of 82 counties are disproportionately black or African-American.
The researchers found that 97 percent of disproportionately black counties reported at least one case of COVID-19, compared to 80 percent of all other counties. Forty-nine percent of these counties reported at least one death, compared to 28 percent all other counties.
The study also looked at health, economic and social factors that are associated with increases in COVID-19 cases and deaths. Investigators found that people who live in disproportionately black counties with more uninsured people and households that are more crowded are at increased risk for acquiring COVID-19.
Millett said that a lack of testing access could mask the true extent of the health disparity.
“African Americans are less likely to be tested for COVID-19, but are also more likely to be diagnosed with COVID-19 if they are tested, so we may be underestimating,” he said.
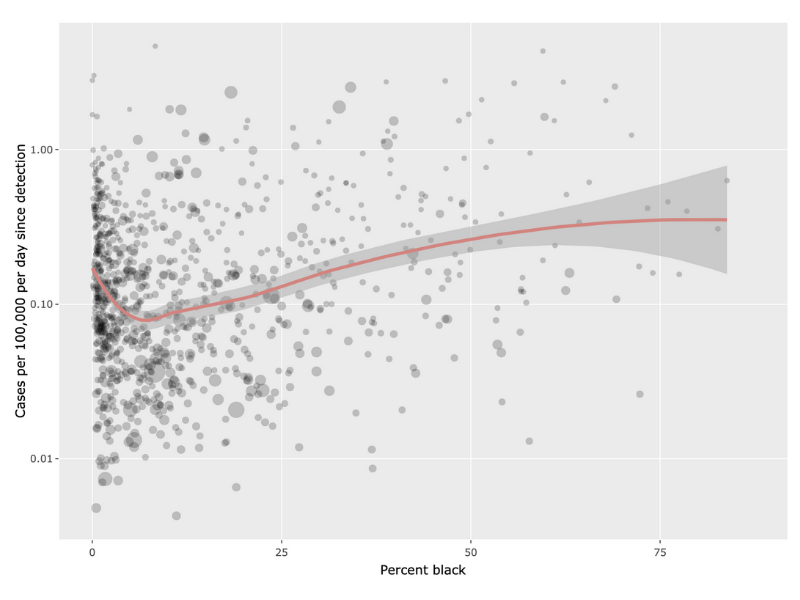
An interactive tool produced by the Foundation for AIDS Research lets users explore county-level data on COVID-19 and race.
Mena said systemic inequalities might make testing harder for African Americans to access testing. For instance, not having a car makes it more difficult to get to a testing site.
The study also showed differing patterns of confirmed cases and confirmed deaths based on geography.
“While COVID-19 cases did not vary dramatically between more urban and rural counties, COVID-19 deaths were greater in rural and small metro disproportionally black counties,” Mena said.
This could be attributable to the “limited health system capacity” in these areas, where rural hospitals have closed on have fewer intensive care beds.
“Most of these rural and small metro disproportionally black counties with increased COVID-19 mortality are in the South,” Mena said. These communities have a higher proportion of uninsured residents in part due to limited Medicaid expansion, he said.
As of May 5, the Mississippi State Department of Health reported 8,207 confirmed COVID-19 cases and 342 deaths. Black African American Mississippians make up 57 percent of cases and deaths, even though they make up only 38 percent of the population.
Mena said that the results from this study reveals three starting points to use as health officials try to reduce COVID-19 mortality, correct their response, and prepare for a second outbreak.
“Increase the proportion of vulnerable Americans that are insured, consider the access challenges experienced by vulnerable populations as we plan testing and hopefully vaccination sites, and be mindful of our communication strategies and messaging,” he said.


