Good oral hygiene can factor in successful surgical outcomes

EDITOR’S NOTE: A version of this story originally appeared in the Fall 2020 edition of Dentistry, the magazine for University of Mississippi School of Dentistry alumni.
When Dr. Jacob Moremen came across a study linking improved oral hygiene to a reduction in post-operative pneumonia for lung and esophageal cancer patients, he had an idea.
Moremen, an assistant professor of surgery and member of the interdisciplinary thoracic team at the University of Mississippi Medical Center Cancer Center and Research Institute, is always looking for ways to improve his patients’ medical outcomes. Because 20 to 40 percent of patients risk some kind of lung infection after surgery, battling pneumonia is a top priority for him.

“Pneumonia is typically the first domino to fall. If you’re going to have subsequent problems (after surgery), it starts with that infection, which can lead to a longer time in the hospital and possibly other infections,” which then leads to even greater issues, Moremen said.
When a person undergoes anesthesia for surgery, there’s an increased incidence of aspiration, or breathing foreign materials into the airways. The risk of aspiration is what’s behind the common recommendation for patients not to eat anything after midnight the day of surgery.
“Normal people aspirate every day, but we have good mechanisms, like coughing, and healthy immune systems protect us,” Moremen explained.
But when someone’s put under anesthesia – especially someone who’s immunocompromised – their defenses are lowered, leading to risk of a complicated aspiration. The study Moremen reviewed showed improved oral hygiene could make a positive impact on a patient’s results after surgery, likely because of a decrease in bacteria in the mouth and, as a result, a decrease in bacteria being aspirated during and soon after surgery.
He linked up with Dr. Sandra Horne, professor of dental hygiene in the University of Mississippi School of Dentistry, and soon their own research study was born. Horne helped secure dental supplies at a reduced cost, and they were able to start offering patients packages with toothbrushes, dental floss and other hygiene items.

Beginning in fall 2019, students in the dental hygiene program were stationed in the Thoracic Oncology clinic. The students visit patients, many of whom had just learned of their cancer diagnosis, to assess their oral hygiene and provide education. They document the patients’ plaque index, offer oral hygiene education and provide the package of supplies, with the goal that patients’ oral hygiene improves before surgery, usually scheduled for around two weeks later.
“The students will teach oral education to the patient, such as how to correctly take care of their teeth and mouth, if he or she feels comfortable,” said Horne, noting that if the patient declines to participate, they are given written materials to view later. “We want our students to develop skills to be empathetic toward these patients, because they’re in a state of having had trauma. The lessons they learn here will improve their delivery of oral health care to future patients.”
During the appointment, students explain that while topics such as teeth brushing and flossing could seem trivial given their recent news, improved oral hygiene could have a major impact on the success of their upcoming surgery.
They use disclosing solution to change the color of the patient’s plaque and highlight trouble areas. The student can then show the patient those areas and educate them about correct teeth brushing, dental flossing and tongue cleaning.
Two weeks later and prior to the patient’s surgery, dental hygiene faculty will re-assess the patient’s plaque index and other oral hygiene indicators. They then record that data for the research study.
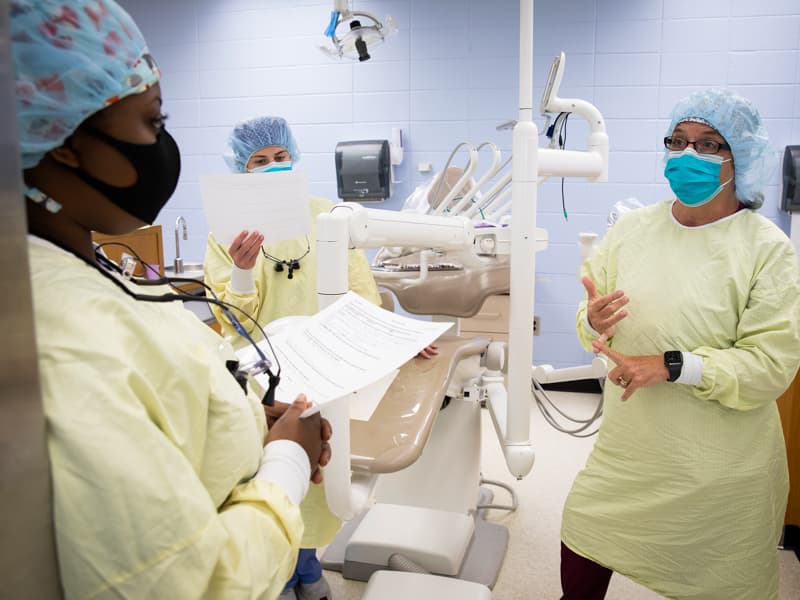
Ellie Roberts, a graduate of the dental hygiene program who rotated through Moremen’s clinic, said the experience was unique.
“I learned that it goes such a long way in health care and in life in general to be kind and understanding of people,” she said. “I always explained to the patients that I can only imagine what ‘I’m going to take you to the next room to go over oral hygiene’ could seem like after receiving the news of a difficult diagnosis.”
She and her fellow students always sought to be as empathetic as possible while sharing with patients the science behind why oral hygiene is especially important as they face surgery.
“I tried to show them I truly do care and want them to have the best chance possible at a successful surgery and full recovery,” she said.
Although the project was halted for several months because of the COVID-19 pandemic, members of both departments are already thinking how they can collaborate more in the future.
“It’s really opened our eyes to where we can further develop this because it’s becoming very evident that these patients need their teeth cleaned before surgery,” Horne said.
The partnership offers the Department of Surgery a unique chance to work on a big problem using a different approach. “It’s easy to keep banging away at the same stuff: more masks, cleaner instruments, faster surgery,” Moremen said.
He feels confident in this out-of-the-box approach.
“We want to make thoracic cancer surgery as low risk as we can, and this is an area for risk reduction and quality improvement.”


