Pancreas-kidney transplant ends years of suffering for Delta resident
Tim Murphree has never felt so good.
Diagnosed at age 11 with insulin-dependent diabetes, the Mississippi Delta native was sick for years before that. “I lost a lot of weight in the seventh grade,” he said. “I’d dealt with it so long that feeling bad seemed normal, like it was the way it was supposed to be.”
As he approaches 48, feeling good is becoming Murphree’s new norm. A pancreas-kidney transplant at the University of Mississippi Medical Center on June 4 – just two weeks after his name went on an organ waiting list – leaves him free of his insulin pump, free of constantly painful dialysis, and free of worrying how long he’ll be around to care for the 16-year-old daughter he’s raised as a single parent.
He is free, Murphree says, “to do something else.
“I don’t want it to end. This feels so good,” said Murphree, who lives in tiny Tippo in rural Tallahatchie County. “My doctors have told me not to work out, but this is the first time in my life that I’ve had enough muscle mass to do it.”

Dr. James Wynn, professor of transplant surgery, performed the six-plus hour procedure that came after Murphree began dialysis in February. He had a catheter required for the procedure surgically implanted at a Memphis hospital.
Thirty-six years of fighting diabetes had taken its toll on Murphree, who despite his disease, he said, never missed work during the five years he was employed as a technologist at a clinic before his transplant.
Dialysis was a rotten temporary fix for a chronic problem.
“It pulled 32 pounds off me,” at a time when he was already thin, Murphree said. “I didn’t realize how bad I looked. There were complications from the catheter surgery, and it was installed at the wrong angle. It was hurting so bad. I had a lot of sleepless nights.”

Her dad endured a number of serious diabetic episodes over the past couple of years, said Amelia, a high school junior. “Dialysis did not help him at all. It was really bad. He was really bony.”
“One time, my blood sugar was out of whack and she was trying to get sugar in my mouth. I was out of my mind,” Murphree remembered. “Amelia called my uncle, and they took me to the ER at 4 in the morning. She was with me the whole time, and she had school in the morning.”
He didn’t know, Murphree said, that the solution to his advancing disease was in his own backyard. A simultaneous pancreas-kidney transplant is often the last hope for a person with type 1 diabetes, which results when the pancreas can no longer make enough insulin, a hormone that regulates the absorption of sugar into a person’s cells. That causes blood sugar to rise to harmful levels.
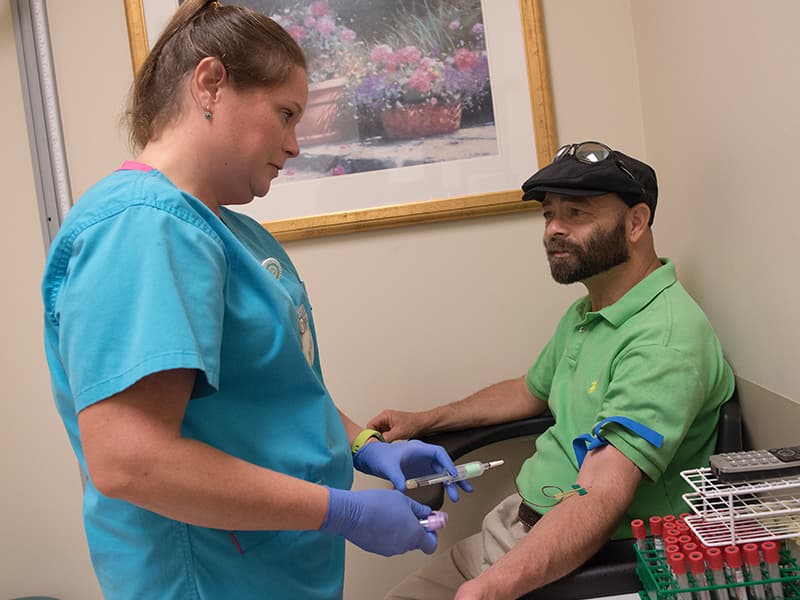
“The group I was seeing in Memphis needed a blood test, and I asked if I could just have it done in Grenada and have the results sent to them,” Murphree said. He went to UMMC Grenada, about 30 minutes down the road from Tippo, to get his blood drawn.
He saw a flyer at the laboratory inviting patients to a transplant class led by Michelle Crawford, a registered nurse and abdominal transplant coordinator at the hospital’s transplant clinic, a satellite of the Division of Transplant and Hepatobiliary Surgery on UMMC’s Jackson campus. A transplant surgeon staffs the clinic on the third Friday of the month, each time seeing an average 12 new patients needing transplants and an average five receiving post-transplant care.

Crawford gave him referral paperwork needed for a transplant evaluation by UMMC. “He had no idea he would qualify for a pancreas-kidney transplant, and didn’t know we offered these services,” she said. “It felt like a divine intervention to me personally.”
Murphree said he thought he’d be lucky if he got a transplant in the next five years. “You’re going to fly through this,” he said Audrey Williamson, an old friend and nurse at the Grenada clinic, told him.
She was right, but the timing could have been a lot better.
His 92-year-old grandmother had recently suffered a stroke. In the midst of that, Crawford surprised him with the good news that he’d made it onto the transplant waiting list. Two weeks later, Murphree put Amelia on a plane for a much-anticipated trip to visit friends in Chicago. His grandmother was still hospitalized.
The next day at about 3:45 a.m., Murphree’s cell phone rang. “I didn’t want to answer. It said ‘unknown,’’’ he said. But, he did.
“It was a lady from UMMC. She said that they had a pancreas and kidney for me, and if I was ready to accept it, I needed to be there at 8 in the morning. My daughter was with friends and that was a blessing, but my grandmother had just had a stroke,” he said. “My granny has a dog, and I have a dog, and all of a sudden my daughter wasn’t in town to feed them.”
He called his uncle, who lives next door and who had agreed to be his designated support during the procedure, and asked him to drive him to UMMC. Murphree found a friend to take care of the dogs.
When he got to the Medical Center, Murphree said, he’d steeled himself to be disappointed. What if the organs weren’t a match after all? What if something went wrong and the surgery was called off?
“But there was no hesitancy,” he said. “My goodness, I was ready. I was ready to get off dialysis. I’d been sick all my life, but with dialysis it was non-stop.”
During his surgery, Murphree’s aunt and uncle stayed in the patient room reserved for him. “They got lots of calls, back and forth, telling them how I was doing in surgery,” Murphree said.
Amelia said she didn’t worry about her dad. “I wasn’t scared,” she said. “I had faith. I had people at my church praying for him.”
“I woke up, and by that afternoon, I was walking the halls. I was eating by Sunday afternoon,” Murphree said. When he got home five or six days later, “my daughter was in the driveway, waiting for me.
“I never thought I could have kids. Other than my transplant, Amelia is the only successful thing in my life. She’s a wonderful person. She makes you a better person.”
Murphree said he’s gaining back his strength and seriously considering a job offer. “I could never have imagined it would have been as nice as it was,” he said of his transplant experience.
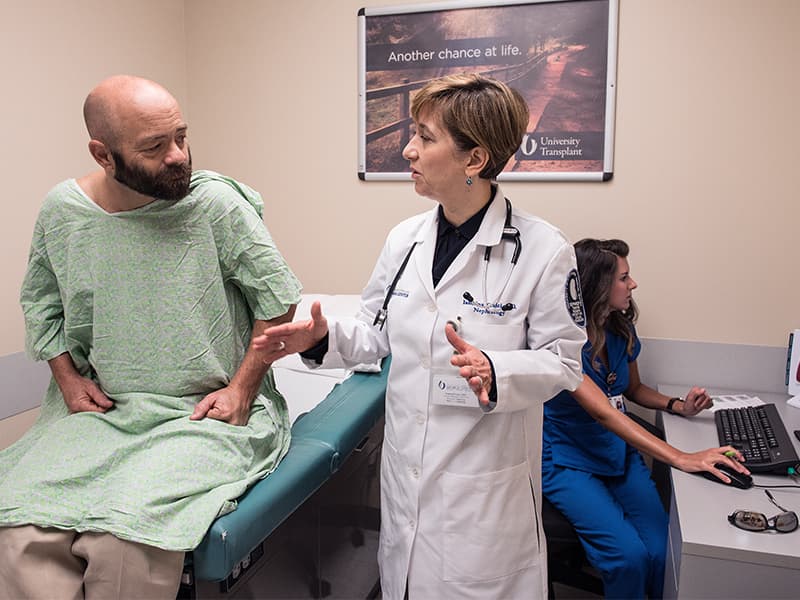
His first post-transplant trip to see a nephrologist was Sept. 7. Murphree met with multiple members of his care team, including Dr. Iasmina Craici, associate professor of nephrology; nurse practitioner Steve Harvey; and his transplant coordinator, registered nurse Kristen Turnbow.
“You’re normal now,” Harvey told him after asking him if he’d had abdominal pain, night sweats or other symptoms. “Be smart and drink water all the time, but from a surgical perspective, you’re an A-plus.”
“Your amylase and your sugar look perfect,” Craici said after giving him a physical exam and reviewing his bloodwork.
Murphree is planning a celebratory cruise with Amelia later this fall. “We will just chill,” Amelia said. “My dad’s just a lot happier. He’s always looked sick, but now he looks like he’s glowing.”
“I’m living a little, finally,” Murphree said. “There is no limit to it now.”

