Team care propels UMMC liver transplant program to national honor
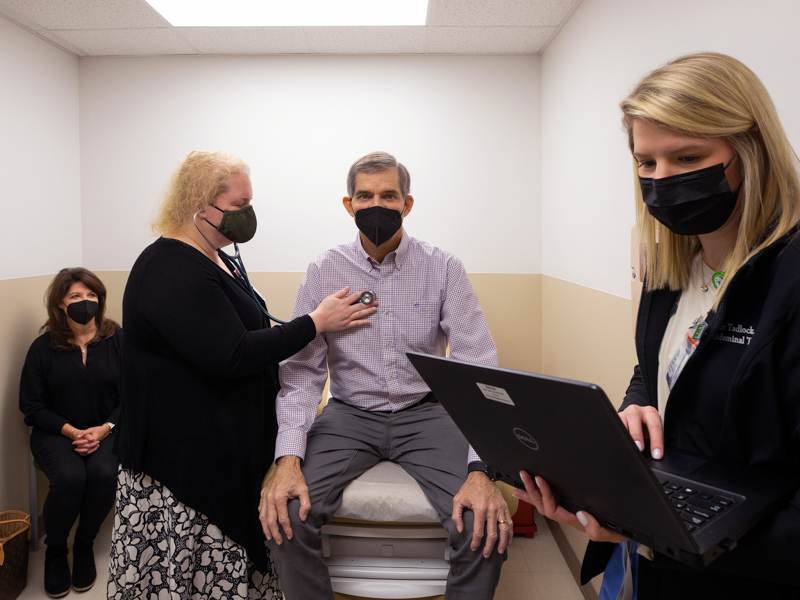
When Randal Russell’s chronic liver disease was diagnosed more than a decade ago, the Madison resident sought care at an out-of-state hospital that offered a liver transplant program.
“But then, they got a program here,” Russell’s wife Sherri said of the University of Mississippi Medical Center, where liver transplants resumed in 2013 after a 20-year hiatus. “We heard lots of really good things about it and felt comfortable switching.”
Fast forward to Sept. 27, 2021. His liver crippled by primary schlerosing cholangitis, a progressive inflammation and scarring of that organ’s bile ducts, Russell had been on a transplant waiting list at UMMC since July 2020 when he got the call: We have a liver for you.
His transplant took place the next day, but treatment on the front and back ends of the surgery has as much to do with survival and recovery as the procedure itself.
That round-the-clock caregiving factors into UMMC’s liver transplant program being listed in the top three in the country by a federally contracted organization that compares transplant centers nationally.

That honor clearly shows that the Medical Center “can aggressively transplant patients and have excellent outcomes,” said Dr. Christopher Anderson, James D. Hardy professor and chair of the Department of Surgery.
The Scientific Registry of Transplant Recipients listed the Medical Center above some significantly larger programs such as the Mayo Clinic hospitals in Jacksonville, Fla., and Phoenix, Barnes-Jewish Hospital in St. Louis and the Ochsner Foundation Hospital in New Orleans.
The registry lists 148 liver transplant centers on factors including one-year post-transplant survival rates, survival rates of patients on a liver transplant wait list, and how fast someone on the waitlist received a deceased donor transplant. The registry also considers how many living and deceased donor liver transplants are performed annually.
UMMC received a score of five out of five on one-year survival and on getting a deceased donor transplant quickly. The Medical Center received three out of five on survival rates of patients while they are still on the liver transplant waiting list.
The Medical Center’s liver transplant surgery team includes Anderson, its leader; Dr. Mark Earl, a professor in the Division of Transplant and Hepatobiliary Surgery and surgical director of liver transplantation; Dr. Felicitas Koller, associate professor in the division; and Dr. Praise Matemavi, assistant professor in the division. Dr. James Wynn, professor in the division, is primary responsible for kidney transplant.

“We’ve got a world-class team, and our outcomes speak to it,” Earl said. “During surgery, our anesthesiologists are very good at keeping very critically ill patients stable, and they can get very sick during transplantation.”
They’re joined in the OR by nurses in addition to surgical and anesthesia techs. “You know you are surrounded by experts,” Earl said. “It allows the surgeons to focus on their job, and their job only.”

The team also includes veteran registered nurses designated as pre-procedure and post-procedure abdominal transplant coordinators. Anna McGraw, Lacey Dungan, Jodie Kilby and Taylor Tadlock guide and monitor patients, getting to know them well and taking responsibility for the smallest details that could affect their recovery and well-being.
Add to that hepatologists, infectious disease specialists, nurse practitioners, psychologists, social workers, pharmacists, dieticians, primary care physicians, even financial coordinators.
“She’s unbelievable. She’s so responsive,” Russell said of McGraw. “That’s the biggest factor for me. She cares. She’s attentive. If there’s an issue, they get it resolved. Dr. Matemavi texts me and checks on me all the time. She’s been great.”
When a patient receives a new liver depends in large part on their Model for End Stage Liver Disease (MELD) score. It ranges from a six, the least ill, to 40, gravely ill. The federal United Network for Organ Sharing uses a formula based on MELD scores to match organs with recipients.
The Medical Center in 2021 performed 48 liver transplants, and since the program restarted in 2013 has completed 333, including several in which two patients shared a single liver.
“We are where we are today because of essentially a decade of persistent dedication to this vision. The earliest of our goals was to be a resource for patients in Mississippi that could provide liver transplant timely and safely,” Anderson said. “At University Transplant, you have a team that is all in and dedicated to the care of liver patients.”
A huge advantage is the transplant hepatology team led by Dr. Laura Smart. “Dr. Smart and the transplant coordinators carry the heavy load and supplement our surgeons perfectly,” said Dean Henderson, transplant services administrator.

“It’s a big factor so far as getting these patients to our clinic and seeing them before they get so sick from liver disease,” said Smart, an assistant professor in the Division of Digestive Diseases. “We keep them as healthy and functional as possible before their transplant.”
She teams with assistant professors Dr. Jan Petrasek and Dr. Joydeep Chakraborty to control issues before transplant that include fluid retention from cirrhosis, bleeding, and challenges with diet and exercise.
“A lot of them have diabetes, hypertension or other conditions that need ongoing monitoring. We also have mental health providers to offer support for depression from chronic diseases,” Smart said.
“Getting a transplant is such a gift. Some people struggle with that.”
The hepatology team provides stellar treatment, “preventing some from needing transplant, and caring for others, some of whom are now nine years post-transplant,” Anderson said.
A patient’s surgery team monitors their care for the first month following transplant. After that, “we see them weekly and space it out as they improve,” Smart said.
On Jan. 19, she visited with Robert Jacobson, a Theodore, Ala., resident who received both a liver and a kidney on Nov. 19, 2021 after being on the waiting list a little over three months. Cirrhosis of the liver and kidney failure caused by chronic diabetes made him a candidate for both.
“My team of doctors has been awesome,” Jacobson said. “In the ICU and on the hospital floor, I got good care, and super care in rehab.”
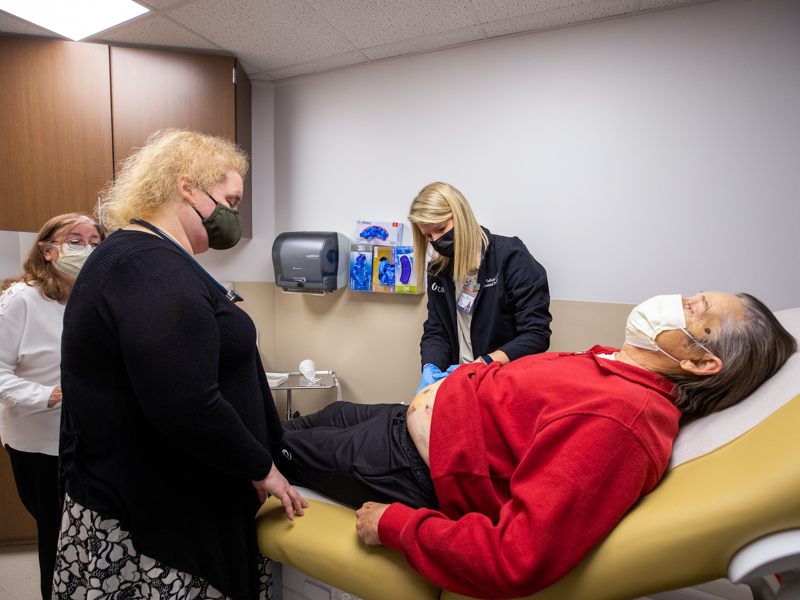
Jacobson chose to drive three hours for transplant care “because they said this place gets a good turnaround,” said his wife Valerie. “We stayed here, and I’m glad we did.”
Every step of the way, a patient’s transplant coordinator is holding their hand – even calling to tell them a donor organ is available.
“Our patients are typically transplanted within a year, and for some, it’s three or four months,” McGraw said. “That’s really fast, and for a liver transplant, you need it to be that fast because patients can be so sick.”
Coordinators before and after surgery keep up with patients’ medications and schedule them for appointments and bloodwork, McGraw said. “We answer their sick calls after hours so that we can take care of their liver as best possible, especially in the face of other diseases.”
“Our nurses have to be pretty top-notch,” Dungan said. “A lot of our patients don’t understand the small details that could mean something is going wrong.”
“We take care of them for the life of the liver,” McGraw said. “We keep them for their entire life.”
“We truly have a great team, with all of the players performing at their top level,” Henderson said. “We have one of the best transplant teams in the country, and now the data is starting to prove that fact.”


