Trauma first target for Neuroscience Institute
Published in News Stories on October 06, 2016
The nervous system is an intricate electrical system, much like a computer. It recalls information, performs calculations on the fly and solves the most complex of problems.
“The nervous system is what allows humans to juggle while riding a unicycle, to envision the ceiling of the Sistine Chapel and contemplate the theory of general relativity,” said Dr. Keith Tansey, professor of neurosurgery and neurobiology and anatomical sciences.
When damaged, the system can go haywire.
“After a spinal cord injury, a patient loses control of movements, but gains muscle spasms. They lose sensation, but gain neuropathic pain,” he said.
Because the nervous system connects to and controls the rest of the body, understanding and caring for this integral system requires an integrated approach. That is the basis of UMMC's new Neuroscience Institute, NSCI for short.

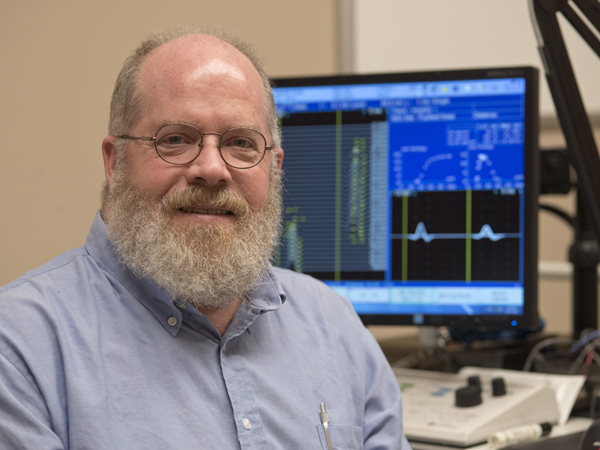
Tansey works in the electrophysiology lab at Methodist Rehabilitation Center.
Approved by the Institutions of Higher Learning in April and operational since July, the NSCI aims to advance clinical care, research and education in three areas: stroke, addictions and neurotrauma. It encourages collaborations across UMMC academic departments, the Adult Hospital and Methodist Rehabilitation Center.
Neurotrauma, including spinal cord and brain injuries, is Tansey's specialty. Dr. Michael Lehman, chair of the NSCI operating board, said he will be one of the leaders expanding existing services into a leading neurotrauma center.
Tansey, who joined the UMMC faculty in February, is also a senior scientist at MRC and a physician at the G.V. “Sonny” Montgomery VA Medical Center in Jackson.

Lehman
“His recruitment represents the collaborative spirit that embodies the institute, which bridges departments and hospitals to help us become leaders in translational research,” said Lehman, professor and chair of neurobiology and anatomical sciences.
In his labs, Tansey studies spinal cord injury, rehabilitation and neuroplasticity, the body's ability to reorganize its neural circuitry after injury.
For example, his 2016 study while at Emory University and the Atlanta VA showed that electrical stimulation and assisted stepping might help augment spinal rhythmic motor output - necessary for walking - in patients with complete spinal cord injuries.
“Using a robotic exoskeletal orthosis over a treadmill, we can manipulate a patient's body and provide gait-related sensory feedback,” even if they have little or no motor control, Tansey said. The machines assist the legs in a walking motion, and the leg muscles respond with small bursts of electrical activity. A technique called electromyography measures these outputs to show how well the muscles respond.
Tansey will continue similar work in MRC's research division, the Center for Neuroscience and Neurologic Recovery.

Stokic
“We use different tools ranging from electrophysiology to kinesiology in order to study the nervous system at multiple levels,” said Dr. Dobrivoje Stokic, senior scientist at MRC and member of the NSCI advisory committee.
One of these tools is the motion analysis and gait lab. Patients walk around the room, their joints and muscles marked by sensors. Cameras focus on the sensors to create a stick-figure-like animation revealing the patient's motion. Reading feedback from the muscles reveals how the nervous system works, Stokic said.
In addition, MRC will expand its research capacity through a NeuroRobotics lab that will open in 2017, enabling similar projects to those Tansey worked on in Atlanta. Both he and Stokic are excited about the opportunities to develop new therapies through research to enhance the recovery of gait, arm use and autonomic functions.
“We are tasked with finding a way to translate these innovations into clinical practice,” Stokic said.
These tests aren't only for research purposes. They are part of the patient's therapy and rehabilitation medicine regimen.
“Physical therapy is moving in a direction where we now see that one size doesn't fit all. Using these tools, we can take a patient's unique profile and tailor therapy based on their abilities,” Stokic said. In turn, he said, “we can assess how well an intervention works.”
The ultimate goal, Tansey and Stokic say, is to improve the continuum of care - and quality of life - for neurotrauma patients.
“If a patient can move from the trauma center to a rehabilitation program faster, with fewer medical complications, this leads to better outcomes and allows the patient to maintain their place in the community,” Tansey said.

In the MRC electrophysiology labs, waves show muscle response to increasing electrical stimulation from an electrode placed behind a patient's knee.
A formal affiliation agreement between UMMC and MRC makes the transition easier. The Neuroscience Institute is another aspect of this affiliation. Since 2014, this collaborative effort has helped the institutions develop well-connected health care for their patients.
The reciprocal relationship formed by the affiliation agreement includes admitting privileges and faculty appointments for clinicians and scientists at both institutions. Later, a new physical medicine and rehabilitation department and residency program will provide more resources to train new physicians and treat more neurotrauma patients.
The ability to affiliate with multiple institutions is a draw for clinicians and scientists such as Tansey, said Lehman.
“[The Neuroscience Institute] is a new way of doing business,” Lehman said. “We are looking for the best people to move us ahead in our understanding of treatments and disease, and we want to figure out how to give these people the best environment for success.”
So far, Tansey said he is impressed with the opportunities in Jackson for translational research and clinical care.
“Many places don't provide the possibility to work in basic science and apply that knowledge to human studies and then to clinical applications,” Tansey said. “It's exciting to come at the beginning of this new collaboration, the Neuroscience Institute, with the possibility to bring all of these resources together.”
Photos
 | High Resolution Medium Resolution Low Resolution |
 | High Resolution Medium Resolution Low Resolution |
 | High Resolution Medium Resolution Low Resolution |
 | High Resolution Medium Resolution Low Resolution |


