If obstructive sleep apnea makes rest elusive, a new device can help
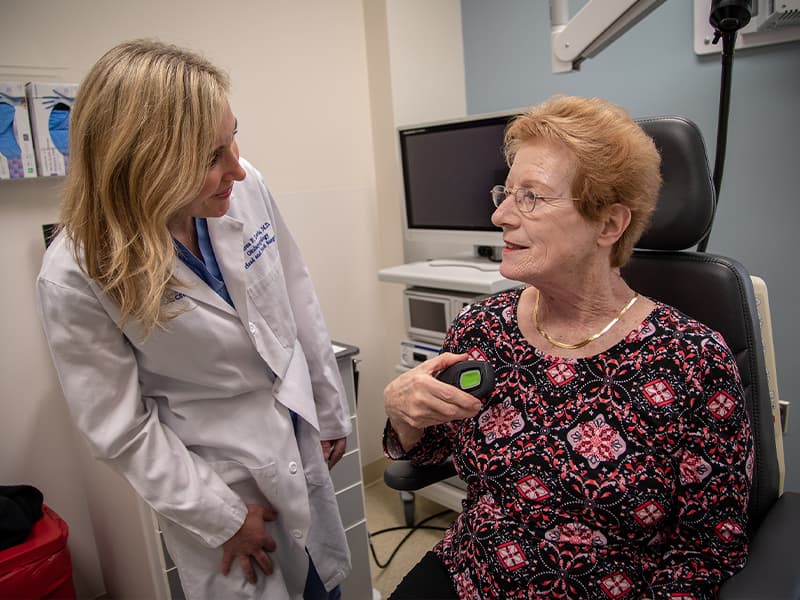
Susan Walters didn’t realize how much sleep she wasn’t getting until her University of Mississippi Medical Center specialist team gave her the therapy to get a full night of restful slumber.
Since the late 1990s, Walters said, “I was waking up several times a night, gasping for breath and snoring. I didn’t think there was anything to it, and that everybody snores.”
Her sister thought otherwise. “She was using a CPAP mask, so I got tested for one,” Walters said of continuous positive airway pressure, a ventilator therapy for sleep apnea patients that uses mild air pressure delivered through a mask to keep airways open.
The CPAP wasn’t for Walters; much newer technology offered by an implant that uses a gentle electric pulse to open up her airway was. “I thought I was sleeping, but I’d get up and feel like I hadn’t rested at all,” she said of the CPAP. “The machine cord was inconvenient when I turned over in the bed. I used a chin strap, and I had to keep my mouth closed and breathe through my nose. It was difficult.”
Walters coped with obstructive sleep apnea, a condition in which a person suffers disrupted sleep and low blood oxygen levels because their tongue is sucked against the back of their throat. That blocks their upper airway, often causing the patient to snore, be unusually sleepy during the day, and sometimes suffer cardiovascular problems, depression or loss of concentration.
Trying to better troubleshoot the problem, 77-year-old Walters underwent a sleep study conducted by Dr. Allen Richert, division chief in the UMMC Department of Psychiatry and Human Behavior and medical director of UMMC’s Sleep Center, located at Select Specialty Hospital in north Jackson.
The majority of studies involve patients spending the night at the Sleep Lab so that their breathing, snoring, movement and oxygen levels can be monitored. Some patients, though, take part in an in-home study that records air flow, oxygen levels and chest movement.

Richert said that the large majority of the sleep studies performed at UMMC are to determine if a patient has obstructive sleep apnea. The most common treatment is CPAP or a newer version of that machine that adjusts during the night. “If the machine notes apnea, it will increase the air pressure on its own,” Richert said.
Richert suggested Walters visit Dr. Andrea Lewis, an associate professor in the Department of Otolaryngology and Communicative Sciences. Lewis determined that Walters was a candidate for a sleep therapy device that delivers mild stimulation to the hypoglossal nerve that controls movement of the tongue and some airway muscles. How much stimulation can be controlled by up and down buttons on a small, hand-held remote control.
Lewis implanted the small device in Walters’ chest as an outpatient procedure, then activated it about a month later after giving the three small incisions time to heal. Walters said she felt immediate relief.
“I was surprised the first time that it worked,” Walters said. “I felt so different when I got up in the morning. I was rested and could stay up later without being drowsy the next day. I realized what I hadn’t been getting all those years.”
The FDA-approved device, designed to provide long-term relief, has a battery life of about 11 years. It works inside the body to address the root causes of obstructive sleep apnea, Lewis said. An electrical impulse delivered to the tongue via a coil running from the hypoglossal nerve to a battery acts much like a pacemaker, she said. A sensor placed between the muscles in the rib area detects when the patient takes a breath, activating a gentle pulse that opens the airway.
“The patient uses a remote control to turn the device on before they go to sleep, and off again after they get up,” Lewis said. “It takes about 30 minutes for it to start working,” which gives the patient time to fall asleep, she said.
The patient hears two beeps when they turn on the remote and a green light shows to indicate it’s been activated, Lewis said. “The patient feels a single pulse on their tongue when it connects,” she said. Patients turn off the device by pressing a gray button, then listening for two beeps. “A status ring on the remote will turn white,” Lewis said.

Walters is among the first patients to receive the implant surgery from Lewis, who began performing it in 2017. Lewis works with patients to find the right setting to give them the best sleep. “You can step up the setting by one level to increase the stimulation, or you can step down if it feels uncomfortable,” she said.
Most patients tend to slowly increase the stimulation during the first two months of use “until they aren’t snoring, or feel that they are sleeping better,” Lewis said. “Some people feel like they get so much benefit that they don’t turn it any higher, but when they have a follow-up sleep study, the find that they could use more.
“The purpose is to find the setting that gives you comfortable sleep,” Lewis said.
UMMC’s sleep team strives to find a solution for all patients, whether it’s the device implanted by Lewis; surgery ranging from removal of tonsils to the more uncommon breaking of the patient’s jaw to move it forward and stretch the face; to CPAP or the use of mouthpieces that hold the mandible forward and mouth closed.
And, weight loss is an important treatment, Richert said. “As the body mass index goes up, the incidence of sleep apnea goes up,” Richert said. “It’s becoming more common. We’re more aware of it.”
Lewis has performed 30-plus procedures, more than any other provider in the state. Lewis has served on the American Academy of Otolaryngology’s national sleep committee and holds certification in sleep medicine from the American Board of Sleep Medicine. UMMC is an ABSM-accredited sleep center.
She’s collecting data at the Medical Center as part of her committee duties. “I was on staff at the University of Pittsburg when this device was originally researched,” said Lewis, who also is a member of the American Academy of Sleep Medicine.
Walters said the device, manufactured by Inspire Medical Systems Inc., has helped her both physically and mentally. The mother of three grown daughters, Walters retired to Clinton after working for 21 years at an insurance company in Ohio.
“I’d fall asleep, but I’d be back up about an hour and a half later with the CPAP,” she said. “Then I’d fall asleep in my chair. This was such a big change.
“I should have done this long ago. I mostly did it to please my sister, but once I found out what a difference it made … She was right.”
To be evaluated for the sleep therapy implant, call the Department of Otolaryngology and Communicative Sciences at (601) 815-0821.


