Therapists restore movement, quality of life to patients with COVID-19
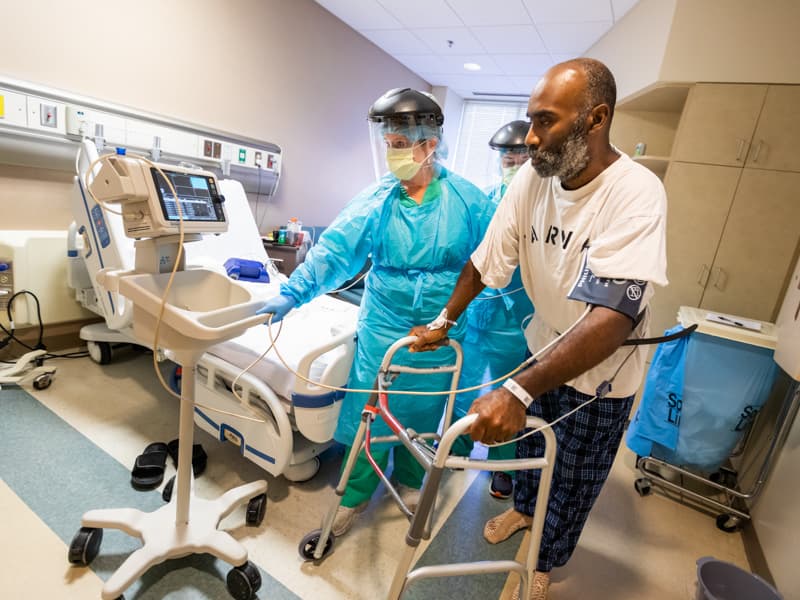
Getting out of bed had never left Terry Doremus frightened to death and gasping for breath.
But in the University of Mississippi Medical Center’s intensive care unit, where the COVID-19 virus nearly required she be placed on a ventilator, the Brookhaven resident was close to panicking as physical therapist Brian Hendley and occupational therapist Charlie Nosco gently worked to help her sit on the side of the bed for the very first time.
“Every time I’d try to move out of a lying position, I’d start losing my breath and coughing,” Doremus remembered of her August hospitalization that stretched for six weeks. “But, they cranked up my oxygen and were patting me and doing all they could do to calm me. They said, ‘Ok, we’re going to sit on the side of the bed, and then that will be it for the day.’

“They were unbelievable.”
When a seriously ill patient with COVID like Doremus turns the corner after days or weeks on their back, it’s cause for celebration and a big sigh of relief.
It also marks another stage in their recovery: Learning to swallow again. Mastering tasks we take for granted, like brushing your hair or taking a shower.
It can be as humbling as making it to the potty chair next to your bed.

“For some, we have to start at the basics of self-care and work our way up,” said occupational therapist Randy Khalaf. “It’s important for us to get them to the point that they can do daily activities on their own.”
Many patients with COVID cope with degrees of “deconditioning” sustained during their illness. It includes muscle weakness and loss of muscle tone; cardiovascular or digestive problems affecting swallowing and movement; and respiratory problems that leave them out of breath.
The Medical Center’s multidisciplinary COVID care includes a much-needed rehabilitation component that encompasses speech and language pathology, respiratory therapy, occupational therapy and physical therapy. Depending on their needs, patients might see multiple therapists and pathologists, as an inpatient or after they’re discharged.
When she woke up in the middle of the night with her throat on fire and a temp of 103, Doremus knew she had the virus.

She’d flown to Texas in late July to help her daughter with her 2-year-old while her daughter recovered from a medical procedure. She arrived at the airport with a headache. “I took Tylenol, and it was better,” Doremus remembered.
That was a Thursday, and the headache lingered. “I get through Sunday, and I don’t feel like myself,” Doremus said. “I was supposed to fly home Monday.”
That didn’t happen. She tested positive, and her husband drove to San Antonio to bring her home. “He didn’t tell me, but he had it, too,” Doremus said. “He didn’t want to worry me.” About a week later, her blood oxygen saturation dangerously low, she was rushed by ambulance to UMMC.

Patients with COVID often need respiratory therapy, said Cody Allen, an adult respiratory therapy supervisor. “They start off with a whole lot of oxygen because they are in so much distress, and we start weaning them off until we can get them to the level of a device that they can take home.”
Help can include non-invasive oxygen therapy such as BiPap, or bilevel positive airway pressure. A BiPap machine uses a mask or nasal plugs connected to a machine that supplies pressurized air to help open up the lungs. “Sometimes, a patient with COVID gets fatigued trying to catch their breath,” Allen said. “This helps them to catch their breath.”
It’s routine for patients recovering from COVID to receive oxygen through a nose cannula, or to build strength with a spirometer. “We may try proning them, or putting them in different positions while they are awake and oriented, to help them with their oxygen,” Allen said.
“You want the healthier part of the lungs facing downward to help with oxygenation. It might be the patient lying on their side, or sitting up,” he said. “Sometimes, we base if off the images we see on their CT scan. Sometimes, it might be that a patient rolled over, and we noticed that their oxygen was much better.”
When a patient is struggling to breathe, their fear can be paralyzing.

“It’s a matter of talking to them, and trying to calm them down,” said respiratory therapy clinical coordinator Levonne Wiley. “You get them to concentrate on their breathing, and you get them to slow it down.”
When patients hear the alarms on respiratory equipment beep, “that can stress them,” Wiley said. “You must tell them that every time they move their finger, the alarm is so sensitive that it might go off.”
“I don’t think I’ve ever seen anyone who wasn’t anxious. I assure my patients and say, ‘I am here for you,’” Allen said. “I tell then we have all the stuff to take care of you.”

When Khalaf and fellow occupational therapist Sacha MacGown assess a patient, how well the person can breathe plays a significant role. “We teach them about having everything they need set out in front of them before they get dressed, and to put their pants on first because it takes the most energy,” MacGown said.
“People can be so debilitated that they can’t do a lot in a short amount of time,” Khalaf said. “I had one lady who was recovering in Wiser. No matter how bad she felt, she always got up and tried to work with us. I always respected her for that.”

Most patients with COVID receiving care from physical therapist Edward Tonos weren’t hospitalized solely for the virus. During his current month-long rotation, Tonos said, “all but one of them came in with other things - maybe they had a wreck or suffered a traumatic injury or fall, and then they were tested and we found out they had COVID.”
That can make their care more complex. “We have to be very careful not to overdo it with them on the acute end, because they are acutely ill,” Tonos said. “They have a hard time getting their oxygen saturation levels above normal.”
On a recent shift, Tonos provided physical therapy treatment to seven patients with COVID. “Some might have had COVID for quite a while, and some might have just been diagnosed,” he said. “We do an activity, and then we let them recover from it. We’re trying to get them to where they are able to function in their house, or in whatever living condition they were in before they came to us.”

Compared to some ICU patients, those with COVID “might be intubated much longer, perhaps two weeks,” said Andrea Lowrie, adult inpatient lead speech-language pathologist. “They have so much longer to be deconditioned. That greatly increases the likelihood that they will have significant swallowing problems once they’re extubated.”
Helping a patient to be comfortable – and safe – in swallowing food and liquids after days or weeks on a respirator or with a tracheostomy is a major part of a speech-language pathologist’s job. The patient’s throat may be sore and raw, and it hurts to swallow. Speech-language pathologists help patients improve their swallow function with strengthening and coordination exercises. They also can play an important role in improving patients’ speech, language and cognitive functions.

“Not being able to eat and drink is a significant quality of life issue. If patients start swallowing and it’s not safe, that can have other serious consequences, such as malnutrition, dehydration, pneumonia or feeding tube dependence,” said Dr. Rinki Desai, adult outpatient lead speech-language pathologist.
“Initially, we might give them a small ice chip to see if they can contain it in their mouth, let it melt down, and swallow it,” Lowrie said. “We palpate their larynx to make sure it’s moving.”
Then, the patient progresses to a sip from a spoon and a low-level diet like liquids or thick liquids. “If they look OK, we allow them to sip from a straw. If a patient is weak or not alert, we might stop and evaluate them later. As they get stronger, we try to upgrade their diet,” Lowrie said.
Doremus’ recovery is going well, although there are bumps in the road. “My lung tests and X-rays still show I need the oxygen,” she said of follow-up care Oct. 7 at the Medical Center. “I did a cognitive test, and I felt like I was failing miserably. We own a business and I keep the books. I can only work on it for so long, and then I hit a wall. It’s really affected me.”
The Medical Center’s therapists and speech-language pathologists are braced for what fall and winter could hold.
“I’ve seen flu cases escalate to someone needing full life support. Sometimes, the flu can be that severe, just like this coronavirus,” Allen said.
“The difference, though, is that I’ve never seen one and a half to two ICUs totally dedicated to the flu. I’ve seen two ICUs dedicated to coronavirus, plus two whole hospital floors.”


