News
- Department of Neurosurgery
- Contact Neurosurgery
-
News
- Department of Neurosurgery News
- 2025
- 2024
- 2023
- 2022
-
2021
- Patient Story: Bradley Hamblin - Brain Tumor
- Patient Story: James Irwin - Childhood Cancer
- Patient Story: Judy Herrington - Stroke
- Patient Story: Kathleen Keeton - Spine
- Patient Story: Lee Roy Nail - Trigeminal Neuralgia
- Patient Story: Patrick Kerns - Aneurysm
- Patient Story: Paul Miller - Pituitary Tumor
- Patient Story: Tamika Larkin-Stowers - Epilepsy
- A Year Later
- New Technology for Minimally Invasive Procedures
- Minimally invasive procedure repairs brain aneurysms at high risk of bursting
- Patient Stories
- About the Department
- Education
- Research
- Support the Department of Neurosurgery
Patient Stories
 The Saga of the Christmas Pajamas: Raymond Sinele's Road to Recovery
The Saga of the Christmas Pajamas: Raymond Sinele's Road to Recovery
When Beverly Sinele packed for a holiday trip to Panama City, Florida, she had a specific wish: to spend a cozy weekend away from home in matching Christmas pajamas with her husband Raymond.
She ultimately got exactly what she wanted, though certainly not in the way she expected.
For the Sineles, Christmas 2024 was supposed to be a relaxing start to their retirement with a trip in their RV. The couple enjoyed a quiet walk by the beach, a nice meal and an evening to themselves. Unfortunately, their calm holiday plans changed in an instant.

Healing with Humor: Hannah’s Journey After Spinal Cord Injury
"It's weird to love a hospital so much, but when they've done so much for you, you can't help but love them," says Hannah Evans Johnston, 27, from Carthage, Mississippi. Meeting Hannah today, with her bright smile and positive energy, it’s easy to overlook the fact that she is partially paralyzed. It’s even harder to imagine the severe spinal cord injury that changed her life just over a year ago.

Healing Together: The Tindle Family's Story of Survival and St
rength
After a devastating car accident in 2023 left 17-year-old Marlee Tindle fighting for her life, her remarkable journey to recovery started with UMMC neurosurgeon Dr. Allison Strickland. But the Tindle family’s challenges weren’t over. Less than a year later, Marlee’s mother, Kaky, discovered a potentially life-threatening brain aneurysm. Once again, the family turned to Dr. Strickland for expert care. Their story of resilience and the skilled support they received highlights the profound impact of UMMC’s Neurosurgery team. Read their inspiring journey of hope and healing!

From Courtroom to Comeback: Prosecutor's Journey After Spinal Injury
In the blink of an eye, everything can change. For 34-year-old prosecutor and youth soccer coach Amanda Sturniolo Langford, that moment arrived on April 8, 2024, when her car was rear-ended at a stoplight in Greenwood, Mississippi, triggering a four-car pile-up. The sickening crunch of metal and the brief chaos that followed lasted only seconds, but the aftermath threatened to alter her life forever.
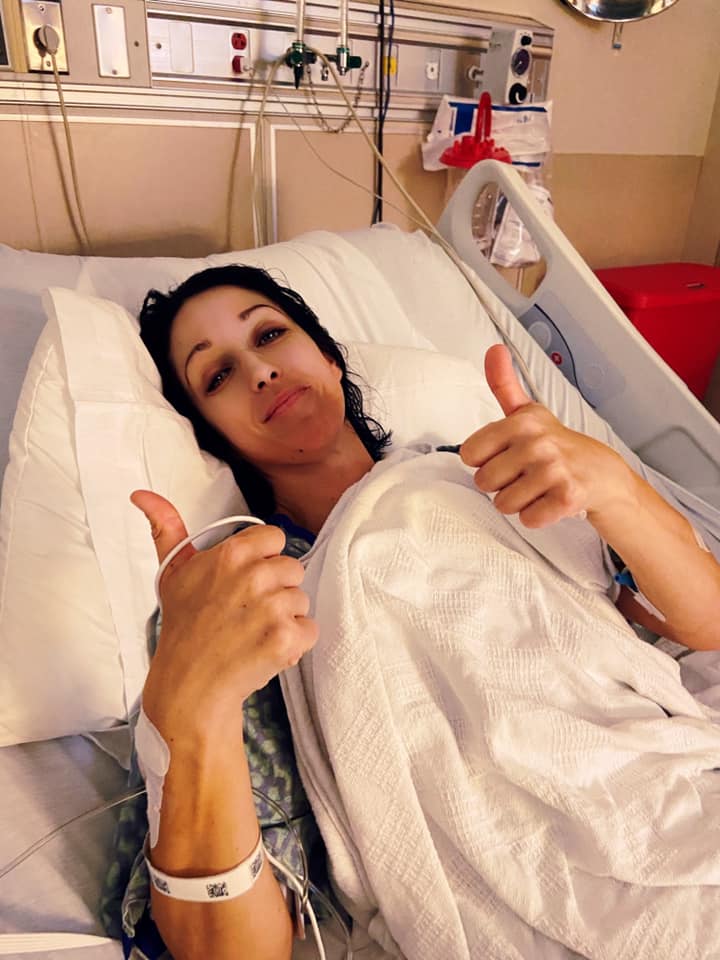
Innovative Treatment Leaves Little To No Deficits
One week after her fortieth birthday, Maggie Slusarczyk, a Polish woman living in Madison, Mississippi, found herself lying on her front lawn unable to speak or move. That morning she woke up with a terrible headache, but got her two boys off to school and sent her husband on his way. She began getting ready for work when suddenly she heard a popping noise in her head and could feel warm pressure spilling over. She called her husband and said, “something is happening to me. I don’t think I’m going to make it. I think I’m dying.” He immediately turned around to drive home. She called 911 and started telling them her symptoms, but her speech became garbled. She stumbled outside for fresh air and then collapsed in her front yard. Though she faded in and out of consciousness, she remembers the paramedics and her husband arriving at the same time. They loaded her in the ambulance as she tried to scream that her head was killing her. She was taken to the University of Mississippi Medical Center for a stroke.
Morgan Richardson - Spine Tumor 
Morgan Richardson of Greenwood MS, a nurse with two children under the age of five, thought her back and leg pain came from long workdays and the rigors of parenthood. After months of discomfort and treatment for sciatica, she went for an MRI at Greenwood Leflore Hospital. Imaging revealed a complicated mass on her spine.
Epilepsy Surgery Inspires Hope 
Driving down the highway, Tamika Larkin-Stowers went from laughing with her cousin to suddenly waking up to the sound of truck horns and panic in her cousin’s voice. She barely had time to swerve off the road to avoid a major collision and had no idea what just happened to her. This was her first experience having a noticeable seizure and the timing almost took her life.
Lee Roy Nail - Trigeminal Neuralgia
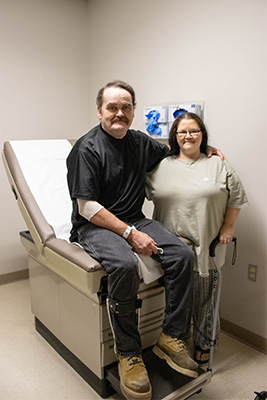 Imagine excruciating pain every time you put a mask on, brush your teeth, or even kiss your spouse. Lee Roy Nail of Stewart, Mississippi, lived that pain for years. With a constant sensation of burning from his eyebrow all the way down to his chin and across to his ear, the pain was so bad that he couldn’t shave. His beard was so long that his kids and their friends referred to him as “lumberjack.”
Imagine excruciating pain every time you put a mask on, brush your teeth, or even kiss your spouse. Lee Roy Nail of Stewart, Mississippi, lived that pain for years. With a constant sensation of burning from his eyebrow all the way down to his chin and across to his ear, the pain was so bad that he couldn’t shave. His beard was so long that his kids and their friends referred to him as “lumberjack.”
Nail tried everything to reduce his agony. Dental work didn’t help, medications didn’t last. “I don’t know how many doctors we went to,” said Nail’s wife, Karol. “One of them even told us it was all in his head! That he was making up the pain in his mind.”
Minimally Invasive, Innovative Procedure Repairs Aneurysms
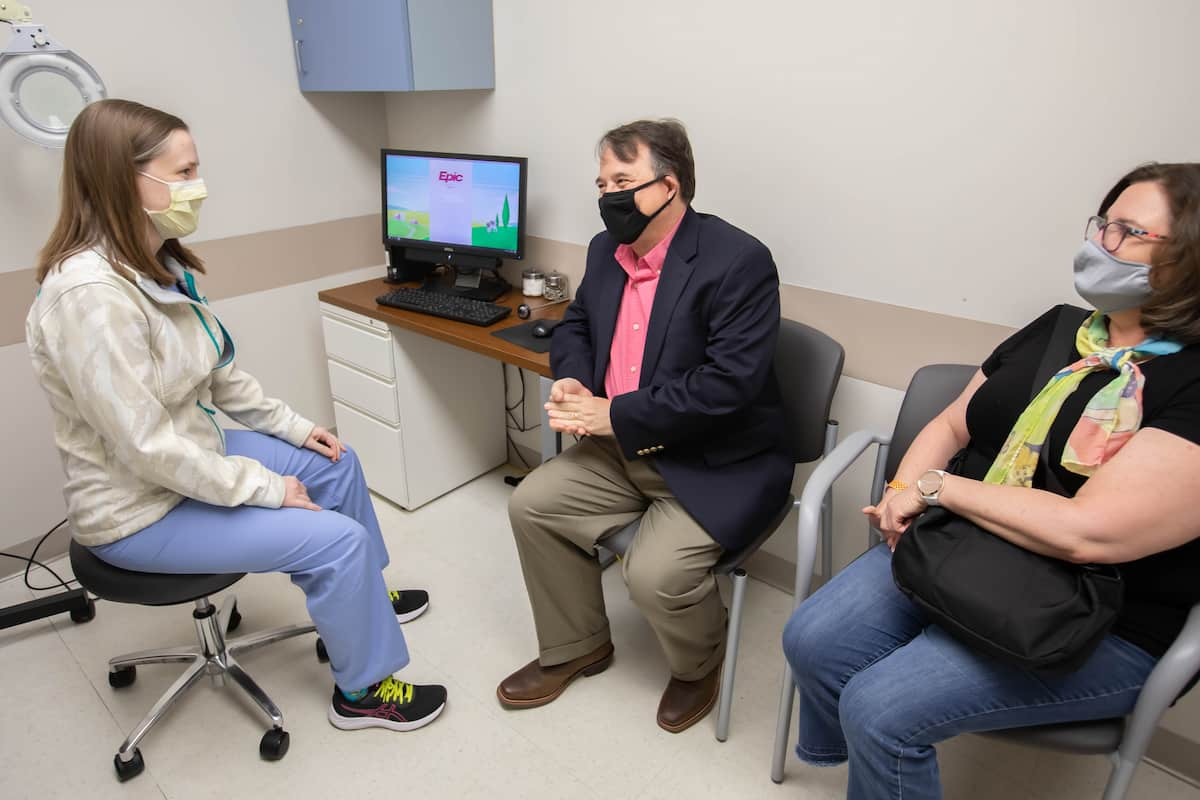 When Patrick Kerns had a stroke on Feb. 9, his CT scan at the University of Mississippi Medical Center revealed a brain bleed that could have killed him.
When Patrick Kerns had a stroke on Feb. 9, his CT scan at the University of Mississippi Medical Center revealed a brain bleed that could have killed him.
If that wasn’t enough, the scans showed an unexpected and not necessarily related problem: an aneurysm of his right internal carotid artery, a major artery that carries blood to the brain.
Nothing Short of a Miracle
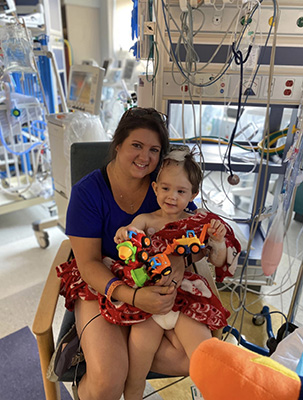 When we decided to start a family, we had no idea what was in store for us. After not being able to get pregnant on our own, and after a few failed attempts at other procedures, we decided to try IVF, which luckily succeeded in the very first round. 32 weeks later we welcomed our baby boy, James, into the world. We were so happy to finally bring him home after his three-week stay in the NICU. Little did we know what was waiting around the corner for him. Our son, who already had a rough start in life, would soon face a scary brain cancer diagnosis.
When we decided to start a family, we had no idea what was in store for us. After not being able to get pregnant on our own, and after a few failed attempts at other procedures, we decided to try IVF, which luckily succeeded in the very first round. 32 weeks later we welcomed our baby boy, James, into the world. We were so happy to finally bring him home after his three-week stay in the NICU. Little did we know what was waiting around the corner for him. Our son, who already had a rough start in life, would soon face a scary brain cancer diagnosis.
Paul Miller - Pituitary Tumor

“The staff at UMMC literally and figuratively saved my life.” Paul Miller, 38 of Horn Lake, received emergent surgery at the University of Mississippi Medical Center in November of 2020 and he couldn't be more grateful.
In 2014, Miller was diagnosed with a pituitary brain tumor. He opted for brain surgery outside of Mississippi. He first received a trans labial resection, a procedure to remove as much of the tumor as possible through his nose, then received radiation to shrink what remained. Able to carry on with his regular lifestyle, Miller lived on his own, worked, and helped take care of his family with minimal difficulties for several years.
Judy Herrington – Acute Ischemic Stroke Survivor
 On July 5, 2019, Judy Herrington, a 60-year-old physical therapist from Madison, was scheduled to have her cardiac pacemaker’s battery replaced at the University of Mississippi Medical Center. “It was a routine outpatient procedure, so I didn’t feel the need to ask anyone to accompany me,” said Judy. “I thought I would be in and out that same day.” Little did Judy know she would be at the hospital for four days recovering from an acute ischemic stroke.
On July 5, 2019, Judy Herrington, a 60-year-old physical therapist from Madison, was scheduled to have her cardiac pacemaker’s battery replaced at the University of Mississippi Medical Center. “It was a routine outpatient procedure, so I didn’t feel the need to ask anyone to accompany me,” said Judy. “I thought I would be in and out that same day.” Little did Judy know she would be at the hospital for four days recovering from an acute ischemic stroke.
Bradley Hamblin – Awake Craniotomy for Brain Tumor
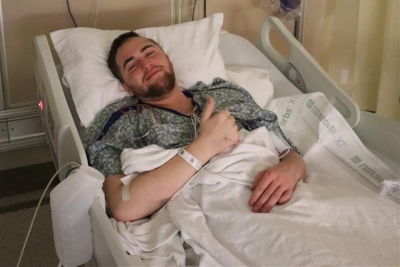
Bradley Hamblin, a 24-year-old from Dennis, was having continuous headaches that by September of 2020, had turned into severe migraines. Thinking it might be related to his eyeglass prescription, he made an appointment to see an optometrist. His eye exam revealed a swollen optic nerve that sent him to the emergency room for further evaluation. “I went to the ER at North Mississippi Medical Center in Tupelo,” Bradley said. “They did a CT scan that showed a large mass, and so they ordered an MRI which indicated I had a brain tumor.”
Kathleen Keeton – Lumbar Stenosis with Neurogenic Claudication
 Kathleen Keeton, a 79-year-old from Jackson, has a long history of back pain. She first underwent back surgery in 2012, followed by hip and knee replacement. Following the surgeries, she was able to resume most of her normal activities including walking with a cane for stability and driving. In late 2019, Dr. Chad Washington, Chair of the Department of Neurosurgery, treated her with steroids for lumbar stenosis, a narrowing of the spinal canal. She seemed fine until December, when she began having excruciating lower back pain and difficulty walking.
Kathleen Keeton, a 79-year-old from Jackson, has a long history of back pain. She first underwent back surgery in 2012, followed by hip and knee replacement. Following the surgeries, she was able to resume most of her normal activities including walking with a cane for stability and driving. In late 2019, Dr. Chad Washington, Chair of the Department of Neurosurgery, treated her with steroids for lumbar stenosis, a narrowing of the spinal canal. She seemed fine until December, when she began having excruciating lower back pain and difficulty walking.


